Introduction
Candidiasis1 of the vulva and/or the vagina is very common in women, giving a variety of urogenital manifestations. Its synonyms are monilia, moniliasis, Candida vulvovaginitis, vulvar thrush, and yeast infection. It is well known to women, who may assume that any vulvar irritation or discharge is yeast and self-treat, inhibiting ability to track this condition accurately.2 3
Vaginal candidiasis is discussed in Annotation P Vaginal Secretions, pH, Microscopy, and Cultures.
Mucocutaneous vulvar candidiasis with or without vaginal involvement is discussed here.
Epidemiology
The exact incidence of candidiasis is unknown. However, 75 percent of premenopausal women report having had at least one episode of vaginal yeast infection and 45 percent of women have two or more episodes.4 Incidence and prevalence of cutaneous Candida is not known.
Etiology
20-50% of asymptomatic women have the C. albicans organism in their lower genital tracts.5 The majority of symptomatic yeast infections (80-90%)6 are a result of Candida albicans. Less common are the non-albicans species (C. tropicalis and C. glabrata in 25% of cases).
Candida probably reaches the vulva and vagina due to proximity of the rectum, but clearing yeast in the GI tract does not prevent recurrent vulvovaginal infection.7 The complex reasons that women become symptomatic are not completely understood.
Candida is normally present on the skin, and may also be a secondary invader when dermatitis such as intertrigo, severe irritant dermatitis, or dermatosis such as lichen simplex chronicus is present. (Atlas: Intertrigo), (Atlas: Irritant dermatitis), (Atlas: Lichen simplex chronicus).
Factors increasing likelihood of symptomatic infection include the use of some medications, particularly antibiotics, corticosteroids, chemotherapeutic agents, and certain diseases: diabetes and immunodeficiency.
Symptoms and clinical features
The most common complaints are vulvovaginal pruritus, although burning, dysuria and dyspareunia may also be present. Complaint of vaginal discharge varies; discharge is not a hallmark for diagnosis especially if Candida involves only the vulva.
Vulvovaginal candidiasis has several different patterns.
Classic vaginal candidiasis presents with a sudden onset of itching, burning, often with curdy white or yellowish-white vaginal discharge, and dyspareunia, along with dysuria in some cases. The vulva may be erythematous and swollen around the vestibule and labia minora.
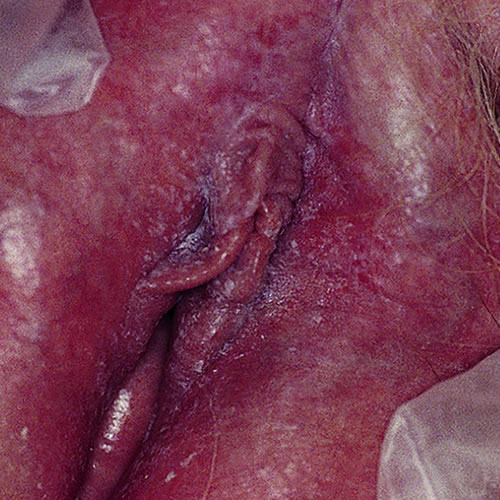
Cutaneous vulvar candidiasis presents with moist, erythematous plaques that can evolve to some degree of erosion. Often typical satellite pustules and peripheral desquamation within the plaques are present. If the condition is very extensive, it can extend up into the crural folds and down onto the thighs. There may be excoriations from scratching.
Eczematous candidiasis causes persistent itching and scratching that leads to thickening of the vulvar skin (lichenification), with excoriations, redness, and chronic swelling. This looks clinically like lichen simplex chronicus or chronic contact dermatitis, showing persistent erythema and swelling around the interlabial sulci and labia minora with some degree of involvement of the labia majora and tiny satellite pustules on the outlying affected areas. Discharge may be scanty or absent.
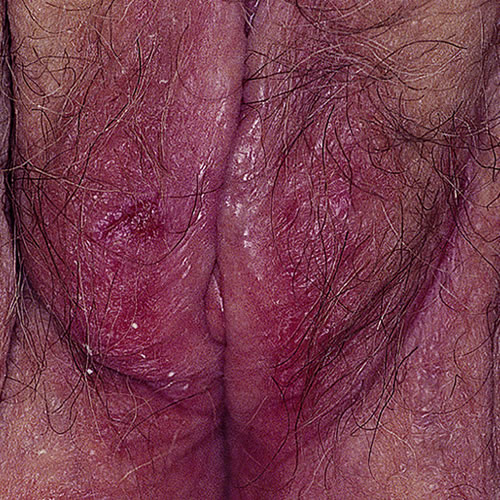
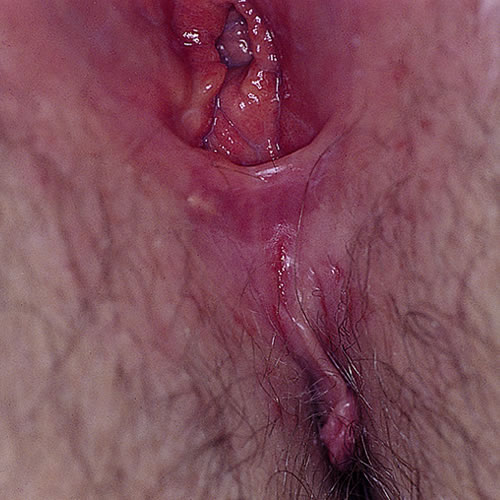
Candidiasis may also cause tiny fissures on the perineum, in the interlabial sulcus, and along the prepuce of the clitoris with pinpoint areas of pain, worse with urination or wiping. There may be a degree of erythema and little to no discharge.
Diagnosis
Diagnosis is clinical with scrutiny of the skin for erythematous plaques and typical satellite pustules, fissuring, or excoriations. With extensive and severe vulvar lesions, the diagnosis of yeast is often missed. Culture is helpful in confirming the diagnosis. Culture can also inform the clinician when yeast is NOT involved, but rather, there is an inflammatory skin condition going on.
Pathology/Laboratory Findings
The vaginal pH is usually 4.5 or less, although yeast infection can occur with an elevated pH. Microscopic examination of skin scrapings mixed with potassium hydroxide 10% may reveal mycelia and budding yeast spores. A yeast culture may be positive. Cultures should be done liberally to both confirm and refute a diagnosis of candidiasis if the pseudohyphae of C. Albicans are not seen on microscopy. Budding yeast spores can be associated with both C. Albicans and non-Albicans strains. (Annotation P, section on candidiasis). Non-Albicans yeast overgrowth tends to be less symptomatic than that of Albicans.
Differential diagnosis
Intertrigo, seborrheic dermatitis, psoriasis, eczema, contact dermatitis, lichen simplex chronicus.
Treatment/management
Control the local symptoms. In all cases, local care with warm or cool water soaks, patting dry, loose clothing, application of cold gel packs and topical xylocaine 5% will be helpful.
Treat the Candida. Topical or oral treatment with any of the imidazole medications can be used, according to the patient’s preference. Most women prefer the ease of oral medication and the standard treatment is fluconazole 150 mg orally on day one and day three. The pt should be informed that fluconazole is slower-acting than the topical preparations, taking up to 48 hours to reduce symptoms, but its effects last up to 72 hours.8 Its side effect profile is low but includes GI intolerance, headache, rash, and transient liver function abnormalities. Fluconazole does interact adversely with some other medications so this should be taken into consideration when prescribing. In addition, in a nationwide cohort study in Denmark, use of oral fluconazole in pregnancy was associated with a statistically significant increased risk of spontaneous abortion compared with risk among unexposed women and women with topical azole exposure in pregnancy. Until more data on the association are available, cautious prescribing of fluconazole in pregnancy may be advisable. Although the risk of stillbirth was not significantly increased, this outcome should be investigated further.9
Any of the topical azole medications may be used, but these may cause secondary burning of which the patient should be aware. With extensive and recurrent involvement of the vulva, a prolonged course of oral fluconazole is recommended. Fluconazole 150 mg orally for two to three sequential doses 72 hours apart is ordered, followed by fluconazole 150 mg orally, weekly for three to six months.
Low potency topical corticosteroids for 48 hours until the antifungal works may be helpful for patients with the eczematous type. Other dermatoses such as lichen simplex chronicus (Atlas: Lichen simplex chronicus) and lichen sclerosus (Atlas: Lichen sclerosus) require specific treatment.
The addition of oral hydroxyzine (25 mg orally at bedtime) (or other antihistamine) at night may also be helpful with itching.
Pregnancy and lactation: Yeast infections are not considered to be harmful in pregnancy but need to be treated if the patient complains of discomfort. The topical imidazoles are the first line medications to use. The shorter imidazole treatments for 1 to 3 days have a lower cure rate than the 7 to 14 day regimens. The one and three-day products can be very irritating if the vulva is raw and burning. This may be avoided with the seven-day formulations. Topical clotrimazole is Pregnancy Category B and vaginal nystatin is Category A. Butoconazole, miconazole, terconazole, fluconazole are Category C. Fluconazole enters the breast milk and needs to be discussed with the pediatrician.
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 135-138.
- Berg AO, Heidrich FE, Fihn SD, et al. Establishing the cause of genitourinary symptoms in women in a family practice: comparison of clinical examination and comprehensive microbiology. JAMA, 1984; 251:620.
- Ferris DG, Nyirjesy P, Sobel JD, et al. Over-the-counter antifungal drug misuse associated with patient-diagnosed vulvovaginal candidiasis. Obstet Gynecol 2002; 99:419.
- Sobel JD. Candida vulvovaginitis. UpToDate, 2012. Wellesley, Massachusetts.
- Goldacre MJ, Watt B, Loudon N, et al. Vaginal microbial flora in normal young women. Br Med J, 1979;1:1450.
- Odds, FC. Candida and candidosis: a review and bibliography, 2nd ed, Bailliere Tindall, London 1988: 124.
- Sobel JD. Candida vulvovaginitis. UpToDate, 2012. Wellesley, Massachusetts
- Hoang ET, Chappatte O, Byrne D, et al. Fluconazole levels in plasma and vaginal secretions of patients after a 150 mg single oral dose and rate of eradication of infection in vaginal candidiasis. Antimicrob Agents Chemother 1990; 34:909.
- Ditte Mølgaard-Nielsen, MSc; Henrik Svanström, PhD; Mads Melbye, MD, DrMedSci; Anders Hviid, MSc, DrMedSci; Björn Pasternak, MD, PhD. Association Between Use of Oral Fluconazole During Pregnancy and Risk of Spontaneous Abortion and Stillbirth. JAMA. 2016;315(1):58-67. doi:10.1001/jama.2015.17844