Annotation A: The Vulvovaginal Patient
Click here for Key Points to AnnotationWho is the vulvovaginal patient?
In the ambulatory primary care setting, “vulvovaginitis” and vaginal discharge are common presenting complaints, resulting in over 10 million physician office visits annually.1 2
These numbers are only a partial reflection of the myriad visits across all specialties for other vulvovaginal complaints for which statistics do not exist. Many women suffer but do not call, trying to self-diagnose and self-treat, further limiting understanding about the prevalence of the problem. Self-diagnosis3 and treatment by telephone4 have not been found to be accurate or helpful.
Women continue these practices because of the inherent embarrassment of having to present with these issues. Constraints on time for visits, availability of visits and childcare, and hopes for a “quick fix” or spontaneous dissipation of symptoms contribute to attempts at self-diagnosis and treatment. In the United States and around the world, lack of adequate training in vulvovaginal care in medical schools and residencies leads to a paucity of clinicians who are familiar with vulvovaginal problems. Without the tools to accurately diagnose and treat, they often perpetuate the misery that many women experience by continuing treatment for the wrong condition, such as repetitive “yeast infections” or recurrent “bacterial vaginosis”. Frequently, women are told that their symptoms are anxiety related, or all in their heads. They are often not treated with gentleness, dignity, or respect.
The vulvar patient suffers alone. Often, she wonders: “It itches, it burns. I can’t have sex. Can anybody help?”
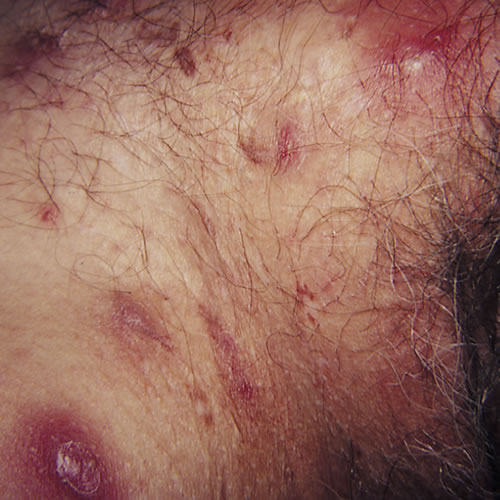
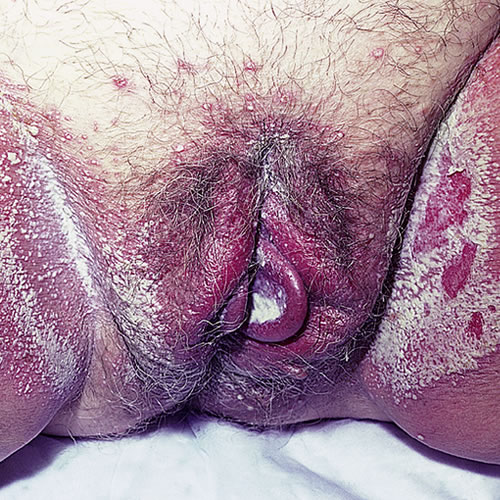
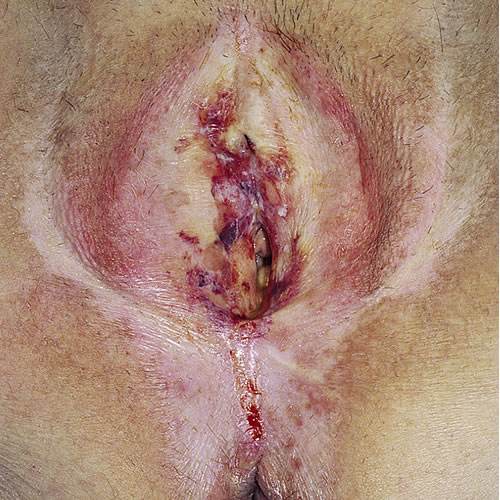
Symptoms of vulvovaginal disease
Pruritis
The most frequent vulvovaginal complaint is pruritis (itching), the hallmark of much vulvovaginal disease. Pruritus may characterize the beginning of disease, appear intermittently, or occur in conjunction with pain in the cases below. What are possible sources for itching?
| Possible sources for vulvovaginal itching |
|---|
| Yeast infection |
| Reactions from irritants and allergens |
| Sexually transmitted infections: herpes, genital warts, trichomoniasis |
| Skin diseases: eczema, psoriasis, lichen sclerosus |
| Systemic diseases: Sjögren, Crohn disease |
| Drug reactions |
| Seminal plasma allergy |
| Pain syndromes |
| Neuropathic conditions (e.g hyperpathic itching) |
| Loss of estrogen |
| Precancerous conditions |
| Skin cancers |
Pruritis and pain
These symptoms may overlap and may be described in a variety ways:
- itching with desire to scratch
- itching with scratching causing soreness
- burning
- stinging
- tingling
- irritation
- constant low-grade awareness of vulva
- soreness
- rawness
- swelling
- dryness
- associations with urination
- associations with defecation
Pain not related to sexual activity
- sharp, knife-like stabbing
- burning pain
- deep, aching pain
- pain with gentle touch on vulva, in vestibule, in vagina
- pain with stronger touch on vulva, in vestibule, in vagina
- pain perceived in pelvis
- pain associated with a known (or unknown) vulvar condition such as herpes or erosive lichen planus
- pain associated with urination
- pain associated with defecation
Some women will complain about feelings of pulling of the pubic hair, “ants crawling under the skin,” (formication), or a feeling of “a tennis ball in the vagina.” Others will point to pain in areas outside of the vagina or vulva.
Dyspareunia (pain with penetrative sex)
- pain with penetrative sex “inside”, usually referring to the vestibule: “stabbed with a knife” or “poked with red hot poker”
- pain with penetration giving the sensation of a wall or obstruction to entry
- pain with thrusting (pain deep in the vagina or “rope-burn” type pain)
- post-coital discomfort, soreness, itching, or pain for hours, days, or longer
- inability to have intercourse or penetration at all because of pain
Discomfort presumed from the vagina
- wetness: may be perspiration (hyperhidrosis), urine, vulvar smegma, vaginal secretions
- increased discharge
- discolored discharge
- irritating discharge
- odor
- bleeding or spotting
Vaginal Discharge
- Women also complain of malodor and discharge, both of which may or may not be present. Women, almost universally, are sensitive about the normalcy of both odor and discharge and may mention either or both when they are not really related to discomfort. (Annotation P: Vaginal secretions, pH, microscopy, and cultures).
Symptom timing
Symptoms can be:
- acute or chronic
- intermittent or persistent
- menstrually-related or not
- triggered (provoked) by touch, physical activity, sexual activity, pressure from clothing, washing, wiping, applying topical substances, or position: sitting, standing, lying, moving.
- untriggered (unprovoked), arising spontaneously.
Signs
“Signs” are physical indicators of an abnormality, as opposed to “symptoms” which are deviations from normal that the patient notices on her own. Clinicians may not recognize a vulvovaginal finding (“sign”) as a problem. They may notice “something not quite right” on routine exam, but take no action because there is no complaint from the patient, or because they are unclear about management. Focusing on the details of both the signs and symptoms will help the clinician develop a keen eye for subtle pathology that will aid in improved diagnosis and management of vulvovaginal conditions.
Signs include:
Anatomical changes
- Scarring or fusion of the prepuce to the glans clitoris
- Absence of the labia minora
- Asymmetry of the labia minora, etc. (Annotation F: The vulvar architecture).
Alterations in color, texture, or integrity of the skin
- Color: red, white, skin-colored, dark brown, blue, purple, and/or yellow changes
- Changes in texture: macules, papules, patches, plaques, pustules, blisters
- Changes in epithelial integrity: fissures, erosions, ulcers, scaling, crusting (Annotation H, the vulvar skin)
[/toggle][/accordian]
It is most helpful to see the patient when she is symptomatic, but, in the case of intermittent problems, this is not always possible. If this is the case, the evaluation process can begin with history and basic exam and the patient can return when symptomatic. No woman is turned away if she is in extreme discomfort or if the situation is not ideal for the exam and she feels she must be seen on an emergency basis.
In preparation for any visit, it is helpful if the patient does not have her period (but we attempt to do the best possible examination even if patient has her menses), and has not had intercourse or douched within the last 24 hours. Ideally, she has employed gentle cleansing with mild soap and fingertips only, and has not “scrubbed” the vulva and vagina just prior to the visit. She should be instructed not to use any products, substances, or prescription or non-prescription topical preparations on the vulva or in the vagina during the two weeks prior to her appointment. She needs to discontinue all antifungals including fluconazole. To help her with itching or burning during the time that she must wait for an appointment, she can use topical Lidocaine ointment 5% during the day, stopping 24 hours before the visit. Cool gel packs and tepid soaks followed by a thin film of plain petrolatum will help.
Along with the patient’s complete history, these signs and symptoms are your first clue as to what is wrong. It is important not to leap to conclusions. Instead, recognize the extensive differential diagnosis of vulvovaginal conditions requiring you to complete the algorithm and come to a diagnosis. While pruritus from Candida may be a primary problem or secondary, related to dermatosis, pruritus may arise from myriad epithelial origins: allergy and irritants, atrophy, neurodermatitis, and hyperpathic nerve fiber activity. While bacterial vaginosis is the leading cause of discharge and odor in the United States, these signs also accompany desquamative inflammatory vaginitis or retained foreign body. Reported odor and discharge may be normal if that determination is made through the steps of pH, wet mount, and microscopy, with appropriate adjunctive testing. The entire evaluation process needs completion before making a diagnosis.
References
- Mengel MB, Schwiebert P. Family Medicine: Ambulatory Care and Prevention, fourth edition; New York City, McGraw-Hill Medical, 2004. 392.
- Granato PA. Vaginitis: clinical and laboratory aspects for diagnosis. Clin Microbiol Newslett 2010:32:111–116.
- Ferris DG, Nyirjesy P, Sobel JD, Soper D, et al. Over-the-counter antifungal drug use associated with patient-diagnosed vulvovaginal candidiasis. Obstet Gynecol. 2002; 99:419-425.
- Allen-Davis JT, Beck A, Parker R, Ellis JI, Polley D. Assessment of vulvovaginal complaints: accuracy of telephone triage and in-office diagnosis. Obstet Gynecol. 2002; 99:18-22.