Introduction
Intertrigo1 is a mechanical inflammatory dermatosis in the skin folds caused by friction, sweating, heat, and occlusion.
Epidemiology
Incidence unknown.
Etiology
The friction of two skin surfaces rubbing together, with the addition of sweat, results in maceration, then dermatitis, fissuring, and secondary infection. Intertrigo is worsened by obesity, tight synthetic clothing, incontinence, and any factors that increase heat, sweating, or wetness in the area. With superinfection from bacteria or yeast normally present on the skin, other conditions may result: mucocutaneous Candida, Erythrasma, Folliculitis.
Symptoms and clinical features
Patients present with itching, burning, and malodor in the labiocrural fold, inguinal fold, and in the fold under the abdominal pannus. Erythema, maceration, fissuring, and sometimes frank weeping may be accompanied by considerable odor.
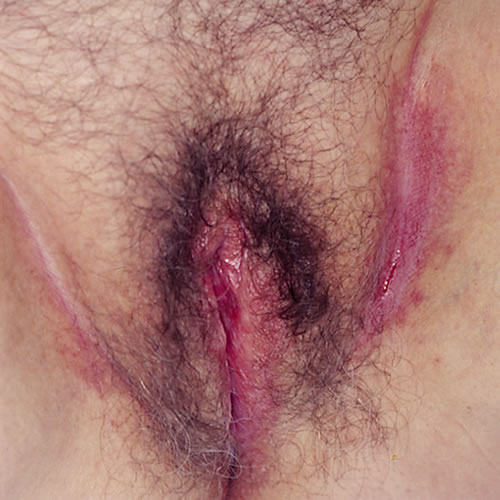
The surrounding skin may show reactive post-inflammatory hyperpigmentation.
Diagnosis
The clinical pattern makes the diagnosis. Bacterial culture and skin scraping for Candida may be helpful. Biopsy should be done if the skin appearance is unusual or does not respond to treatment.
Pathology/Laboratory Findings
There is no specific histopathology.
Differential diagnosis
Differential diagnoses include the following conditions that may be associated with an intertriginous component: psoriasis, seborrheic dermatitis, lichen sclerosus, and familial benign pemphigus (Hailey-Hailey disease).
Treatment/management
The aim is to stop the friction. Patients should avoid tight, hot, synthetic clothing and keep the area cool and dry. Diabetes and obesity should always be aggressively managed.
Reduce sweating with an antiperspirant such as Xerac AC.
Treat bacteria with topical antibiotic such as mupirocin ointment or with oral erythromycin.
Yeast is treated with topical antifungal such as clotrimazole or oral fluconazole.
For mild involvement, gentle cleansing may be all that is necessary. Washing with Cetaphil or chlorhexidine 0.05% solution, rinsing thoroughly, patting the area dry, and using an absorbent powder such as Zeasorb helps to relieve the symptoms. Hydrocortisone 1% powder in miconazole 2% cream can be applied in a thin film as necessary.
A low potency steroid such as hydrocortisone 1% combined with the antibacterial and antifungal action of 10 mg of iodoquinol (Vytone® cream) may work well.
In the groin potent steroid topicals are usually avoided because of the thin epithelium in these areas. Calcineurin inhibitors such as tacrolimus ointment or pimecrolimus cream may also prove effective without risk of atrophy.
For the breakdown under a heavy abdominal pannus, use a thin 100% cotton tea towel or a piece of old sheeting torn into squares. Place against the skin in the fold to absorb the moisture. Change twice a day to stop the friction and prevent recurrences of the problem.