Introduction
Lichen simplex chronicus (LSC)1 of the vulva is the end stage of the itch-scratch-itch cycle, and is a condition well-known to dermatologists. Chronic intense pruritus results in repetitive scratching and rubbing so that the skin becomes thickened in a typical lichenified pattern. The thickened skin itself (epidermal hyperplasia) has a heightened sensitivity to touch which results in itching, relieved only by scratching which is perceived by the patient to bring exquisite relief, if only temporarily.2 In early LSC, generalized erythema may be present before lichenification takes place.
Confusion regarding the overlap in the terms eczema, dermatitis, atopic dermatitis and lichen simplex chronicus is discussed in Eczematous Dermatitis, and is also copied here:
Eczema and atopic dermatitis are synonyms for morphologically and histologically identical skin conditions. Atopy refers to a genetic predisposition for hypersensitive allergic IgE reactions to common environmental antigens,3 with allergic rhinitis (hay fever), asthma, and/or atopic dermatitis that looks exactly like eczema. “Eczematous” refers to the characteristic appearance of the skin. (See eczematous dermatitis.) Atopic individuals may be more likely to develop eczematous skin reactions to common exposures that would not bother the non-atopic person. (Contact dermatitis in the Atlas). (We thus emphasize the important component of vulvovaginal care that stresses the elimination of possible irritants: tight clothing, daily panty liners, panty hose, feminine care products, harsh soaps, or perfumes). At the same time, eczema may occur in those who have no family or personal history of atopy, and atopic dermatitis is rare in the vulvar area.
Lichen simplex chronicus may occur anywhere on the skin, including on the vulva. Itching causes the individual to scratch or rub, exacerbating the itch sensation. The vicious cycle of itching-scratching-rubbing-itching ends up causing the specific morphological condition of LSC: erythema that may occur in plaques of varying depths, in pustules, excoriations, rough scaling that appears shiny rather than flaking, areas of hypopigmentation or hyperpigmentation, especially in people with naturally dark skin. The final hallmark sign of LSC is lichenification: thickening of the skin with the distinctive pattern of normal skin “hatch-markings” being exaggerated and deepened when compared with adjacent, non-affected skin. In addition, because of scratching, hair may be absent or broken. Lichen simplex chronicus may occur because of itching associated with another skin disease such as lichen sclerosus or yeast infection, or may develop as de novo itching.
Histologically, eczema, dermatitis, atopic dermatitis, and lichen simplex chronicus appear the same. A semantic assumption is made by many dermatologists that lichen simplex chronicus is the descriptive term that encompasses localized eczematous conditions in the vulva, atopic dermatitis the term that encompasses generalized conditions, and that the clinician’s job is to come to understand what might have precipitated the condition and treat both the LSC and the originating condition.4
Synonyms for lichen simplex chronicus are hyperplastic dystrophy, neurodermatitis, pruritus vulvae, pruritus ani, and squamous cell hyperplasia.
Epidemiology
While the prevalence of atopic dermatitis is about 15% in Western countries,5 atopic dermatitis, as such, is not common in the vulvar area, while LSC is quite common. Exact prevalence is unknown.
Etiology
Lichen simplex chronicus is the end result of ongoing scratching or the incomplete treatment of eczema, dermatitis or atopic dermatitis, dermatoses, or other conditions.
In primary LSC, the skin is normal at the outset. Irritation from any number of originating causes: yeast infection, reaction to a moisturizer, too-tight clothing, over-washing, panty-liners, sweat, urine, etc, starts the process off. Scratching seems mandatory and pleasurable to patients and may occur in their sleep. If scratching causes extensive excoriation, the woman replaces it with rubbing, which also causes lichenification, and a vicious cycle is set up (the itch-scratch-itch cycle) that must be interrupted to allow healing to take place. The patient experiences stress, itching increases, and persistent habitual scratching (the itch-scratch-itch cycle) results in lichenification and excoriations.6
Secondary LSC of the vulvar skin can occur with associated conditions:
- Infections: Candida, Tinea cruris
- Dermatoses: Lichen sclerosus, atopic dermatitis, psoriasis, contact dermatitis, lichen planus
- Neoplasia: Vulvar intraepithelial neoplasia
- Metabolic conditions: Diabetes, iron deficiency
Symptoms and clinical features
The patient may complain of weeks, months or years of constant itching that is often worse with stress. The skin may initially appear erythematous, without particular lichenification.
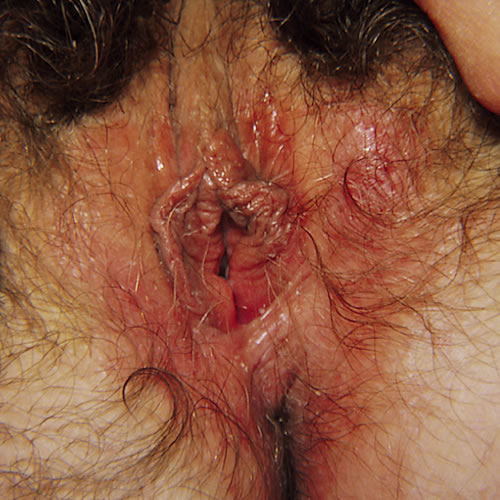
Lichenified skin, in some cases, is like an erogenous zone in which scratching brings pleasure.7 Later, changes in the skin and the seemingly hopeless lack of resolution of symptoms, bring misery. “Nothing helps” and the patient has often seen many physicians seeking answers. Itching awakens patients at night and may also be worse with menstrual periods, heat, and sanitary napkins.
In the secondary lichenification conditions, the condition may arise more quickly, stimulated by the originating insult to the skin.
With LSC, the vulvar skin, particularly over the labia majora, is diffusely thickened, with increased skin markings. This is lichenification.
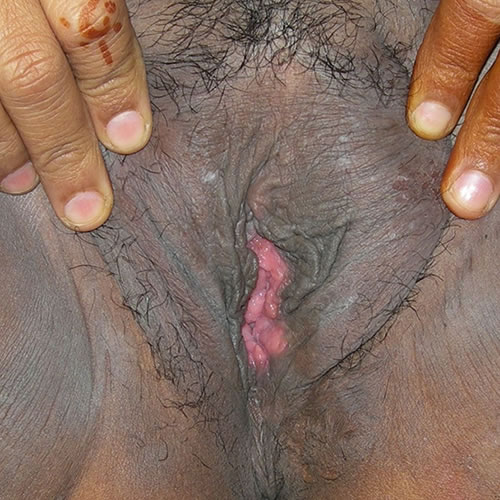
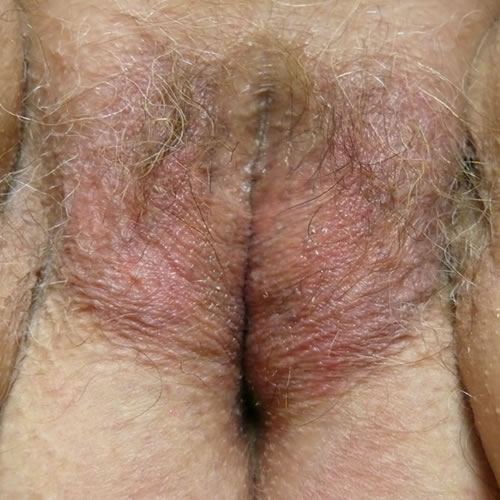
The plaques may be bilaterally symmetric or unilateral, and the skin may be hyperpigmented or hypopigmented. It may show a variety of shades of pink, red, ruddy brown, or purplish, with secondary excoriations (thin, linear erosions caused by scratching), deeper erosions, and crusting.
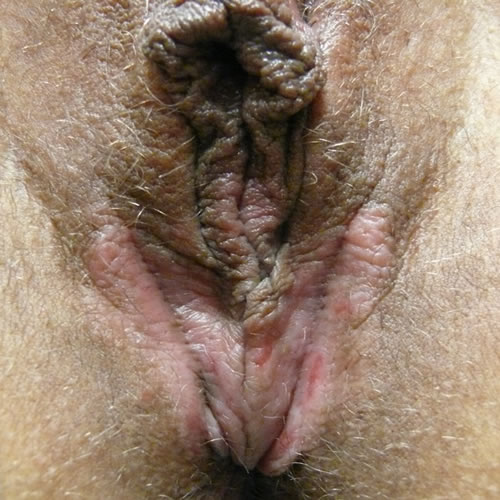
Active rubbing results in considerable swelling and, with time, causes the lichenification and broken off hairs. In dark skin, rather than a solid plaque, closely set papules (follicular pattern) may be seen8 and erythema may be manifested by darkening of the skin (hyperpigmentation) rather than redness.
Pathology/Laboratory Findings
Histologically, hyperkeratosis, acanthosis, a prominent granular layer, and lengthened rete ridges are seen with LSC.9
Biopsy results will often report “psoriasiform dermatitis” or “eczematous dermatitis.” (Psoriasis can occur in the vulvar area and contribute to LSC). Candida must always be ruled out when women report these symptoms because it is often a precipitating factor.
Biopsy can be helpful, at times, in differentiating between LSC and lichen sclerosus, which may also cause itching and hypopigmentation. LSC will not, however, cause loss of the normal vulvar anatomy as will lichen sclerosus.
Diagnosis
Diagnosis is clinical. Biopsy can also make the diagnosis and can rule out other conditions.
Differential diagnosis
Differential diagnosis includes the causes of secondary lichenification listed earlier, and these should be ruled out, since they can all present with this almost identical pattern. Extramammary Paget disease may appear eczematous, like this condition.
Treatment/management
The treatment aim is to stop the chronic itch-scratch-itch cycle.
General therapy:
Control the itch by using:
- Cold gel packs
- Antihistamines — hydroxyzine or doxepin 10 to 25 to 75 mg orally nightly at bedtime, until more comfortable.
Recommend cleansing and clothing practices:
- Warm or tepid soaks are comforting. Gentle cleansing without a washcloth helps. If the condition is mild, use a product such as Cetaphil cleanser or Basis or Dove soap. If the condition is severe, use sitz baths with Burow’s solution.
- Wear cool, ventilated, cotton clothing, and avoid pads if possible.
Specific therapy:
Topical treatment:
- Clobetasol or halobetasol 0.05% ointment: a thin film applied topically twice a day for 2 weeks, once a day for 2 weeks, then Monday, Wednesday, Friday for 2 weeks, then on an intermittent basis, reducing potency for long-term care to desonide 0.05% ointment or 1% hydrocortisone in pramoxine cream.
Intralesional treatment:
- For marked thickness, inject one part triamcinolone acetonide (Kenalog 10) diluted with two parts of normal saline using a 30-gauge needle. The use of EMLA (a topical anesthesia cream applied in a thick film under plastic wrap for 15 to 20 minutes) makes this procedure almost painless. These injections can be repeated at 2 to 3 week intervals.
Infection:
It is necessary to treat any concurrent secondary infections, fungal or bacterial, to help stop the itching. Culture if necessary to rule out superimposed bacterial infection.
These patients need to be seen frequently and given general support. Note: Watch out for combinations of problems, for example, secondarily infected contact dermatitis with underlying psoriasis. Consider patch testing if the patient is not responding.
See table below for details.
Treatment for Lichen Simplex Chronicus
| Treatment action | Topical/behavioral | Oral | Intramuscular | Intralesional |
|---|---|---|---|---|
| Comfort measures, general care | Sitz bath, gentle cleansing, topical petrolatum, avoidance of irritants or tight clothing, application of cool gel packs | |||
| Reduction of itching or pain | Topical xylocaine 5%, applied as needed, usually 4-6 times a day (no more than 15 grams a day) | Hydroxyzine 10 to 25 to 50 mg orally 1-2 hrs prior to bedtime; (may start at 10 mg and increase nightly to a maximum of 75 mg)ORBenadryl 25-50 mg orally 1-2 hrs prior to bedtime, stopping meds as symptoms subdue. | ||
| Anti-inflammatory action | 1% to 2.5% hydrocortisone or desonide 0.05% ointment applied once or twice daily for mild inflammation. This dose may be returned to after more potent steroids have helped.Betamethasone 17-valerate 0.1% ointment applied twice a day in a thin film until improved x 1 monthORTriamcinolone acetonide 0.1% ointment applied twice a day in a thin film until improved x 1 monthORClobetasol or halobetasol 0.05% ointment applied twice a day, in a thin film, tapering with improvement or reducing to one of the previous mid-low potency steroid ointments | Prednisone or methylprednisolone 40-60 mg every morning for 5 days, or a tapering dose up to 7-10 days (for diffuse inflammation, or for those unresponsive to topical treatment | Triamcinolone acetonide 40 mg/ml (Kenalog 40) 1 mg per kg intramuscularly, single dose for diffuse inflammation or for those unresponsive to topical treatment | Triamcinolone acetonide (Kenalog 10), 10 mg/mL diluted 1:1 with saline and using a 30-gauge needle; injected under plaque after application of EMLA (for large, thick areas or those unresponsive to topical treatment) |
| Treatment for candidiasis | Fluconazole 150 mg orally every other day x 3, then weekly until symptoms are gone; for LSC, use in conjunction with steroid treatment. | |||
| Antibiotics for superimposed infection | Dicloxacillin 250-500 mg orally 4 x a day for 10 daysORCephalexin 250-500 mg orally 4 x a day for 10 days | |||
| Reduction of the habit of scratching | Counsel to bring importance of this to patient’s awareness. | SSRIs may be helpful; dosing should start low and slowly build; tapering off the medication should be done very slowly:Fluoxetine (Prozac) 10-20 mg orally, dailyORCitalopram (Celexa) 10-20 mg orally dailyOROther SSRIs |
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 157-159.
- Wolff K, Johnson, RA. Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology, sixth edition. McGraw Hill Medical, 2009. 42.
- Edwards L. and Lynch P. Genital Dermatology Atlas and Manual, third edition. Wolters Kluwer, 2018. p 67
- Edwards L. and Lynch P. Genital Dermatology Atlas and Manual, third edition. Wolters Kluwer, 2018. p 67
- Edwards L. and Lynch P. Genital Dermatology Atlas and Manual, third edition. Wolters Kluwer, 2018. p 67
- Charifa A, Badri T. Harris BW. Lichen Simplex Chronicus in Stat Pearls, Treasure Island (FL): StatPearls Publishing,last updated 7 Aug 2023
- Wolff K, Johnson, RA. Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology, sixth edition. McGraw Hill Medical, 2009. 42.
- Wolff K, Johnson, RA. Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology, sixth edition. McGraw Hill Medical, 2009. 43.
- Heller DS, Wallach RC (ed.) Vulvar Disease: a Clinicopathological Approach. Informa Healthcare USA, Inc., 2007. 61.