Introduction
Painful splits or fissures1 can occur anywhere on the vulva, related to a great variety of conditions. They are not diseases, but rather manifestations of problems in the vulvar skin that may be difficult to sort out.
Epidemiology
Fissures are related to numerous vulvar ailments. The exact incidence is unknown.
Etiology
The etiology of fissures involves the following:
- Infections are the most common cause, Candida most frequently. Herpes simplex can manifest in fissures rather than in the more characteristic blisters and erosions. Beta hemolytic Streptococcus and, infrequently, Staphylococcus aureus are also implicated.
- Dermatoses can result in a dry, scaly surface. Scratching produces painful fissures in psoriasis, lichen sclerosus, lichen simplex chronicus, tinea cruris, contact dermatitis, etc.
- Estrogen deficiency predisposes to thinning of the tissue in the posterior vestibule and commissure. This is usually post-menopausal, but can occur postpartum, especially during lactation, and with some birth control pills.
- There may be fissures in the fourchette related to sexual activity which may be recurrent. It is unclear whether these are simply associated with sexual practices or with an underlying dermatosis, sometimes not yet diagnosed. We have, in our practice, seen at least two cases of young women presenting with fissures in the fourchette as their only complaint, both of whom went on to develop full-blown lichen sclerosus.
- The knife-like fissures related to Crohn disease are usually found in the groin and present, most commonly, as deep ulcers, rather than small fissures.
Symptoms and clinical features
The patient complains of recurrent or persistent painful splits in the vulva.
These tiny, apparently insignificant, fissures cause a disproportionate amount of pain (like paper cuts) and are often missed if not carefully sought.
There may be a history of an itchy “rash” preceding this problem. Clothing, sanitary napkins, and sexual intercourse may be very uncomfortable. Cyclic flaring of the problem before the woman’s menstrual period may occur (as with cyclic Candida infections).
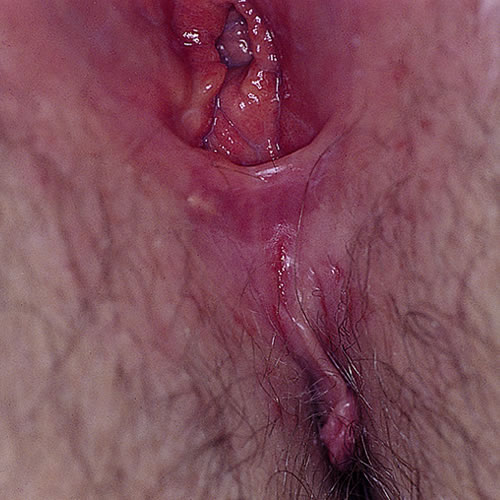
Intercourse may aggravate an area that is dermatitic, causing splitting and possibly precipitating both a Candida infection and further splitting.
If the condition is due to hormonal change, then the history includes onset postpartum, after the initiation of birth control pills or peri or post-menopausally.
The splits are tiny and shallow and rarely longer than 1 cm. In the infections and dermatoses, they are most commonly found in the interlabial sulcus. In the atrophic conditions the splits are in the area of the posterior commissure.
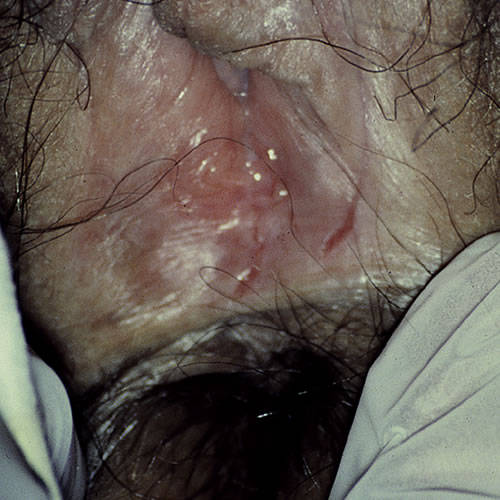
These splits may be accompanied by changes typical of other concurrent conditions such as lichen sclerosus,
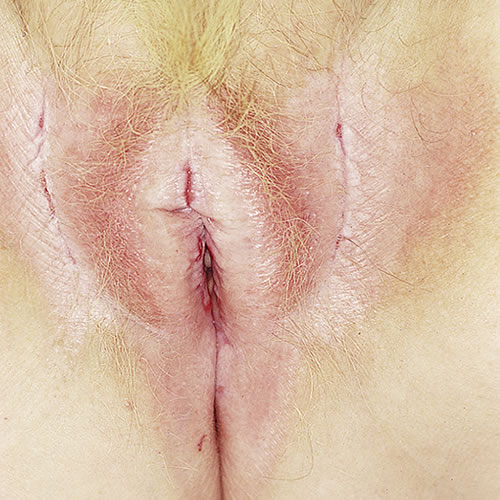
psoriasis, intertrigo.
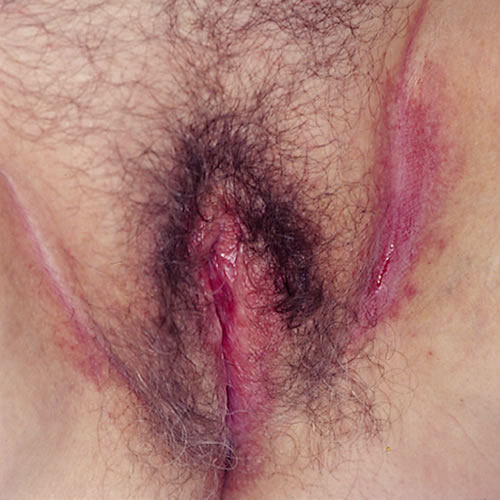
Pathology/Laboratory Findings
Biopsy findings are usually non-specific unless there is underlying disease that can be identified. Yeast culture should be done, as well as any other test that may promote accurate diagnosis, such as herpes culture or PCR.
Diagnosis
The diagnosis is made clinically with the appropriate cultures for infection when indicated.
Differential diagnosis
Candidiasis, herpes simplex, lichen simplex chronicus, lichen sclerosus, atrophy.
Treatment/management
Diagnose the underlying cause of the dermatosis, infection, or atrophy and treat appropriately. The patient should gently cleanse the area with warm water and gentle soap. Instruct the patient to avoid harsh irritating soaps, detergents, sanitary pads, vulvar lubricants, and baby wipes.
- In the case of Candida, suppress with fluconazole 150 mg weekly or clotrimazole 500 mg vaginal suppository for 3-6 months
- Mupirocin ointment applied topically 2 to 3 times a day should be used for bacterial infections.
- Herpes simplex may be suppressed with anti-virals. (Herpes in the Atlas)
- Estrogen deficiency should be treated with a topical conjugated estrogen (Premarin) 0.625 mg/g or estradiol (Estrace) 0.01% cream nightly for 2 to 3 weeks then twice a week as needed.
- Steroid ointment is used to treat lichen sclerosus. (Lichen Sclerosus in the Atlas).
Sometimes simple petroleum jelly applied after cleansing is all that is needed, plus increased lubricant and positional changes during sexual activity. (Lubricants discussion in Annotation P). If it is not possible to correct the fissuring in the posterior commissure, then perineoplasty may need to be considered.