Introduction
Plasma cell vulvitis (PCV), also known as Zoon’s vulvitis and vulvitis circumscipta plasma cellularis, was first described by a dermatologist in Holland in 1952.1 J.J. Zoon had previously described identical pathology of the glans penis: plasma cell balanitis (PCB). PCV, an inflammatory dermatosis, is now thought to exist on a spectrum of plasma cell mucositis, which can involve the oral mucosa (buccal mucosa, lips, palate, gingiva, tongue, epiglottis, larynx) and glans penis (plasma cell balanitis), as well as the mucosa of the vulva.2 Libby Edwards and Peter Lynch, in their excellent reference book Genital Dermatology Atlas and Manual, now exclusively use the term plasma cell mucositis.3 Although many cases of PCB have now been reported, the number of cases of PCV is significantly lower.
Epidemiology
This condition has not been well studied. An extensive recent review of the pertinent and reliable literature determined that, because of a lack of data, no ethnic propensity could be determined. The mean age for patients was 55.3±14.5 years. Prevalence is unknown.4
Etiology
The cause is unknown. PCV does not appear to be a sexually transmitted or infectious disease. Some clinicians believe that it is two different clinical entities: primary Zoon (PZV), arising on a normal vulva and secondary Zoon (SZV) arising in lichen planus or lichen sclerosus.5 Others believe that it is a distinct clinical entity that progresses to lichen planus.6
Symptoms and clinical features
The disease presents as circumscribed, glistening, often rusty-red, solitary or multiple patches or plaques usually in the vulvar vestibule. The areas may be asymptomatic, but are often associated with pain, dyspareunia, or pruritus. The lesions may persist for years or slowly resolve.
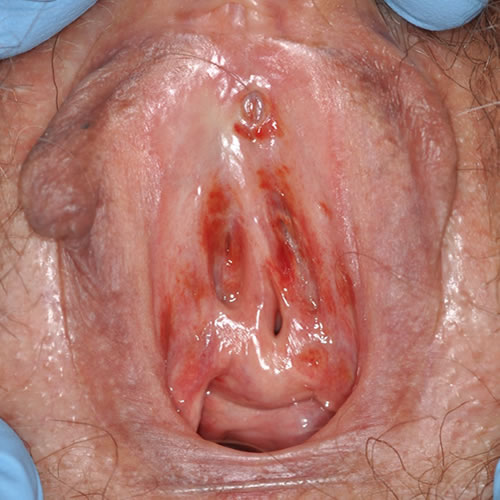
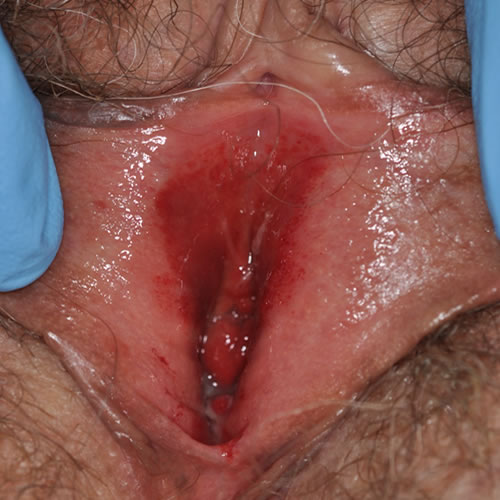
Diagnosis
Diagnosis is based on the characteristic skin lesion and confirmed by biopsy.
Pathology/Laboratory
Biopsy shows an inflammatory infiltrate consisting of predominantly polyclonal plasma cells, along with lozenge or diamond-shaped keratinocytes and erythrocyte extravasation or hemosiderin deposition.7 In one histopathologic review of vulvar dermatology cases, including 15 cases of PCV, basal keratinocyte crowding was identified as a new finding in 86.7% of cases.[efn-note]Chan M.P., Zimarowski M.J. Vulvar dermatoses: A histopathologic review and classification of 183 cases. J Cutan Pathol. 2015;42(8):510–518.[/efn_note]
Differential diagnosis
Erosive candidiasis, VIN, carcinoma, lichen planus, lichen sclerosus, extra-mammary Paget disease, fixed drug eruption, and psoriasis on moist skin.
Treatment/management
Topical mid- to ultrapotent corticosteroids, followed by tacrolimus 0.1% ointment, are the most frequently reported treatments. However, information regarding duration of therapy, treatment time to resolution or recurrence, and measure of treatment efficacy is limited and variable.9
3. Intralesional corticosteroids,10 imiquimod 11 12 and CO2 laser13 are also discussed as helpful in case reports.
References
- Zoon JJ. Differential diagnosis between chronic circumscribed benign plasmacellular balanitis and Queyrat’s erythroplasia. Ned Tijdschr Geneeskd. 1952;96(38):2349–2353.
- Brix WK, Nassau SR, Patterson JW, et al. Idiopathic lymphoplasmacellular mucositis-dermatitis. J Cutan Pathol. 2010;37(4):426–431
- Edwards L and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer, 2018: 98
- Sattler S, Elsensohn AN, Mauskar MM, Kraus CN. Plasma cell vulvitis: A systematic review. Int J Womens Dermatol. 2021 May 4;7(5Part B):756-762. doi: 10.1016/j.ijwd.2021.04.005. PMID: 35028377; PMCID: PMC8714578.
- Wendling J, Plantier F, Berville S, Moyal Barracco M. Zoon’s vulvitis encompasses two different clinical entities: A review of 35 cases. Abstract presented at the XXI World Congress of the International Society for the Study of Vulvovaginal Disease. September 3-8, 2011, Paris, France.
- Selva-Nayagam PA, Olsson A, James CI. Plasma cell vulvitis: Is it a unique entity? Abstract presented at the XXI World Congress of the International Society for the Study of Vulvovaginal Disease, September 3-8, 2011, Paris, France.
- Virgili A., Levratti A., Marzola A., Corazza M. Retrospective histopathologic reevaluation of 18 cases of plasma cell vulvitis. J Reprod Med Obstet Gynecol. 2005;50(1):3–7.
- Virgili A., Borghi A., Minghetti S., Corazza M. Comparative study on topical immunomodulatory and anti-inflammatory treatments for plasma cell vulvitis: Long-term efficacy and safety. J Eur Acad Dermatology Venereol. 2015;29(3):507–514.[/efn-note]
1. Potent topical corticosteroid such as clobetasol 0.05% ointment in a thin film, nightly for 30 days, followed by re-evaluation.
2. Topical pimecrolimus 0.1% (Elidel) or tacroliumus (Protopic) 0.1% nightly for 30 days, followed by re-evaluation. Reports on success vary.8Virgili A, Mantovani L, Lauiola MM, et al. Tacrolimus 0.1% ointment: is it really effective in plasma cell vulvitis? Report of four cases. Dermatology. 2008; 216:243-246.
- Tseng JT, Cheng CJ, Lee WR, et al. Plasma-cell chelitis: successful treatment with intralesional injections of corticosteroids. Clin Exp Dermatol. 2009; 34:174-177.
- Ee HL, Yosipovitch G, Chan R, Ong BH. Resolution of vulvitis circumscripta plasmacellularis with topical imiquimod: two case reports. Br J Dermatol. 2003; 149:638-641.
- Frega A, Rech F, French D. Imiquimod treatment of vulvitis circumscripta plasmacellularis. Int J Gynecol Obstet. 2006; 95:161-162.
- Retamar RA, Kien MC, Chouela EN. Zoon’s balanitis: presentation of 15 patients, five treated with a carbon dioxide laser. Int J Dermatol. 2003; 42:305-307.