Introduction
Vitiligo1 is an acquired loss of pigmentation. It results in irregularly shaped patches of hypomelanosis and/or depigmentation of the skin.
Epidemiology
Affects all races; equal in both sexes; occurs in 1% of the worldwide population.
The incidence of vulvar vitiligo is unknown.
Etiology
Vitiligo is probably an autoimmune disorder, with a polygenic familial predisposition and positive family history of 30%. It is associated with other autoimmune conditions such as pernicious anemia and Addison’s disease, thyroid disease and diabetes mellitus. Environmental exposures, in some cases, may cause depigmentation that resembles vitiligo. There may be an intrinsic melanocyte dysfunction leading to death and/or dysfunction of melanocytes in the lesions.
Symptoms and clinical features
The patient develops a gradually increasing, asymptomatic, sharply demarcated, white area, without textural change in the skin. The cosmetic defect is emotionally traumatic for people with naturally darker skin.
White macules (5 mm to 5 cm or more in size)2 appear most commonly over the extensor areas of the body, most usually at sites of trauma or naturally more pigmented areas of the skin, including the backs of the hands, face, and body folds, including the genito-crural area in women. As the macules enlarge into spreading patches, the hair in the involved area also turns white, helping to differentiate the condition from lichen sclerosus.
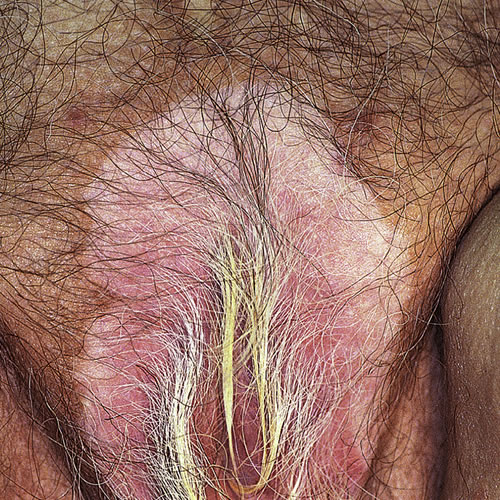
The pigmented area surrounding the outer edges of the whitened skin, may be slightly darker in color than the rest of the normal skin. Scaling, thickening, crusting or skin breakdown are not characteristic of vitiligo.
Patients seen in vulvar clinics may present solely with vitiligo limited to the genital area.
Diagnosis
Diagnosis is clinical.
Pathology/Laboratory Findings
Biopsy, which may show an absence of melanocytes and melanin on special staining, would only be done if the diagnosis was in doubt.
Differential diagnosis
Differential diagnosis includes lichen sclerosus, post-inflammatory hypopigmentation, piebaldism, and lupus erythematosus. Vitiligo may appear together with lichen sclerosus. Post-inflammatory hypopigmentation creates lightened patches of skin but the white is not as strikingly white as vitiligo may be. Vitiligo-like changes may also occur from topical use of Imiquimod, used for treating warts.3
Treatment/management
Treatment of vitiligo is difficult and often disappointing. For involvement of the vulvar area alone, no treatment may be recommended other than reassurance. A dermatologist is needed to supervise a two-month trial of topical mild potency to mid-potency corticosteroids but steroid atrophy can occur if these are over-used, especially in the keratinized skin of the crural folds or labia majora. For extensive disease, topical or systemic psoralens and other therapies such as topical calcineurin inhibitors are being used, but these would not be recommended for localized vulvar vitiligo.
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 194.
- Wolff K, Johnson RA. Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology, sixth edition. McGraw Hill Medical 2009. 335.
- Serrao VV, Paris FR, Feio AB. Genital vitiligo-like depigmentation following use of imiquimod 5% cream. Eur J Dermatol. 2008;18: 342-343.