Introduction
Seborrheic keratoses1 are very common, benign, warty-surfaced pigmented growths that can appear anywhere on the body, but uncommonly on the vulva. Synonyms for this condition are seborrheic wart and senile keratosis.
Epidemiology
Slightly more common and extensive in males, these lesions do not appear until the age of 30 and vary in number from a single lesion to multiple lesions (hundreds) in some elderly people. In females, they may occur more often in the submammary intertriginous skin.2
Etiology
A disorder of keratinocytes, the cause of seborrheic keratoses is unknown but is related to genetics and aging. Because the lesions are common on sun-exposed areas such as the back, arms, face, and neck, ultraviolet light may play a role. However, they are also found on skin that has not been exposed to the sun. A mutation of a gene coding for a growth factor receptor (FGFR3), has been associated with seborrheic keratosis.3
Symptoms and clinical features
The lesions are usually asymptomatic. Occasionally they are itchy and, if scratched, can become secondarily infected. Often, the patient points out the growth, worrying about it being a wart.
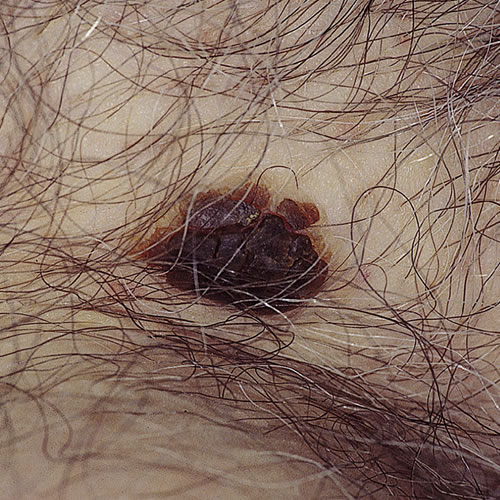
The lesions are 0.25 to 1 cm in diameter and oval to round. They can be scattered anywhere on the lower abdomen and inner thighs or on the non-mucosal surface of the vulva. The lesions are tan colored to brownish black. Their surface may be almost smooth to frankly warty, with a somewhat “stuck on” appearance.
Diagnosis
Diagnosis is clinical and histopathologic.
Pathology/Laboratory Findings
On biopsy, which is only necessary if the diagnosis is in doubt, there is hyperkeratosis, acanthosis, papillomatosis and intraepidermal horn cyst formation.4
Differential diagnosis
Differential diagnosis includes pigmented basal cell carcinoma, melanoma, viral warts, pigmented condyloma accuminata, and pigmented intraepithelial neoplasia.
Treatment/management
Asymptomatic lesions need no treatment. Local destruction can be carried out using electrodesiccation, curettage, shave removal, or cryotherapy.
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 208.
- Wolff K and Johnson RA. Fitzpatrick’s Color Atlas & Synopsis of Clinical Dermatology, sixth edition. McGraw Hill Medical, 2009. 215-216.
- Hafner C, Hartmann A, Vogt T. FGFR3 mutations in epidermal nevi and seborrheic keratoses: lessons from urothelium and skin. J Invest Dermatol. 2007 Jul;127(7):1572-1573.
- Heller DS and Wallach RC. Vulvar disease: a clinicopathological approach. Informa Healthcare, 2007. 146.