Introduction
This benign vascular tumor of the skin or mucous membranes occurs rarely in the vulvar area. Because it occurs more commonly in pregnant women, it is sometimes called the tumor of pregnancy.
Epidemiology
Occurring in both males and females, at any age, the peak incidence appears to be in the second and third decade of life.1Mucosal pyogenic granuloma is more common in women than in men.
Etiology
The etiology is unknown, but the lesion is thought to be a reactive, hyperproliferative, vascular response to a variety of stimuli rather than a true hemangioma.2 Trauma may play a role with two studies showing between 7% and 23% history of previous injury in affected individuals.3 4 There is also an association with some medications in people who are affected in the periungual or subungual areas.5
Symptoms and clinical features
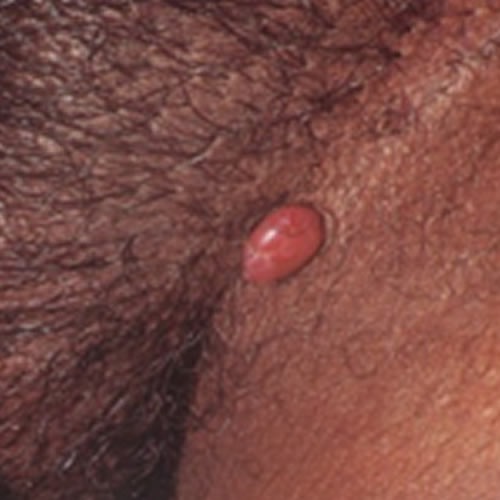
The patient complains of a “bump” that is not tender unless irritated by clothing or catching onto something, in which case, the lesion may bleed. The pedunculated nodules are deep red in color and covered by thin epithelium that may appear shiny or eroded. The lesions may appear as single or as multiple nodules, ranging in size from a few millimeters to a few centimeters,6 and tend to grow quickly.
Diagnosis
Diagnosis is made clinically, on the basis of a history of a red, dome-shaped lesion developing over a number of days or weeks, and is confirmed by histology done on the excised nodule.
Pathology/Laboratory Findings
Pathology shows a polypoid lesion with lobular arrangement of capillaries at the base and a flat, atrophic, sometime ulcerated epidermis. An epithelial “collarette” is described at the base of the lesion if it is cutaneous. The lesion is covered by a single layer of endothelium. Fibroblasts, mast cells, lymphocytes, plasma cells, and polymorphonuclear leukocytes may also be seen, as may edema and inflammation in areas that are irritated.7
Differential Diagnosis
Differential diagnosis includes hidradenoma papilliferum, Kaposi’s sarcoma, basal or squamous cell carcinoma, and amelanotic melanoma. Histology should always be done on these lesions.
Treatment/management
Shave excision of the lesion followed by electrocautery is the preferred method of treatment.8 Recurrence is possible.
References
- Harris MN, Desai R, Chuang Ty, et al. Lobular capillary hemangiomas: an epidemiologic report with emphasis on cutaneous lesions. J Am Acad Dermatol. 2000; 42:1012.
- Requena L, Sangueza OP. Cutaneous vascular proliferations. Part II. Hyperplasias and benign neoplasms. J Am Acad Dermatol. 1997;37:887–919.
- Pagliai KA, Cohen BA. Pyogenic granuloma in children. Pediatr Dermatol. 2004; 21:10.
- Patrice SJ, WissK, Mulliken JB. Pyogenic granuloma (lobular capillary hemangioma): a clinicopathologic study of 178 cases. Pediatr Dermatol. 1991; 8:267.
- Piraccini BM, Bellavista S, Misciali C, et al. Periungual and subungual pyogenic granuloma. Br j Dermatol. 2010; 163: 941.
- Somesh G, Bishan DR, Bhushan K. Multiple, genital lobular capillary haemangioma (pyogenic granuloma) in a young woman: a diagnostic puzzle. Sex Transm Infect. 2000; 76: 51-52.
- Lawley LP. Pyogenic granuloma (Lobular capillary hemangioma). In UptoDate, 2012; UptoDate, Waltham, MA.
- Lynch PJ. In Red Papules and Nodules, in Lynch PJ and Edwards L, ed. Genital Dermatology Atlas, 2nd edition. 2011; Wolters Kluwer/Lippincott, Williams, and Wilkins. 90.