Introduction
Psoriasis1 is a common, hereditary, papulosquamous disease of the skin characterized on the skin surface by typical well-defined, reddish papules and plaques with a silvery white scale. In the inguinal areas the characteristic scale may be missing, a variant called psoriasis inversus or flexural psoriasis.
Epidemiology
Incidence and prevalence for vulvar psoriasis is not known. Psoriasis affects 1.5-2% of the population in western countries.2
Etiology
The exact etiology is still speculative. It is a condition of epidermal hyperproliferation and dermal inflammation, probably the result of dysregulation of keratinocyte formation complicated by disordered immunity in genetically predisposed individuals.3 Trauma, whether physical (scratching), chemical (soaps and perfumes), or biologic (bacterial or yeast superinfection) triggers more psoriatic activity, a process known as Koebnerization. The result is rapidly turning over keratinocytes and inflammation.
Symptoms and clinical features
Irritation or itching is the presenting complaint in the vulvar area. The patient may or may not have a history or obvious lesions in the other typical areas of psoriasis — scalp, elbows, knees, ears, and nails. When the perineum and gluteal cleft are involved, fissuring, pain, and burning may occur. Symptoms are made worse with stress, heat, humidity, tight synthetic clothing, and irritating soaps. Some medications such as systemic glucocorticoids, oral lithium, anti-malarial drugs, interferon, and beta adrenergic blockers can cause flares in existing psoriasis or produce a psoriaform drug eruption.4 Smoking, obesity,5 and alcohol are also triggers.6 Cardiovascular disease, inflammatory bowel disease, and osteoporosis have recently been reported to occur more often in this group.7 An increase in autoimmune diseases is also reported.8
The clinical picture is variable. Papulosquamous lesions can be scattered throughout the mons pubis and labia majora areas. In some cases, there are thin, salmon pink lesions of varying size and shape with minor scaling. In other cases, thick confluent plaques cover all of the labia majora and the mons pubis, forming almost a solid horseshoe pattern with a silvery-white adherent scale.
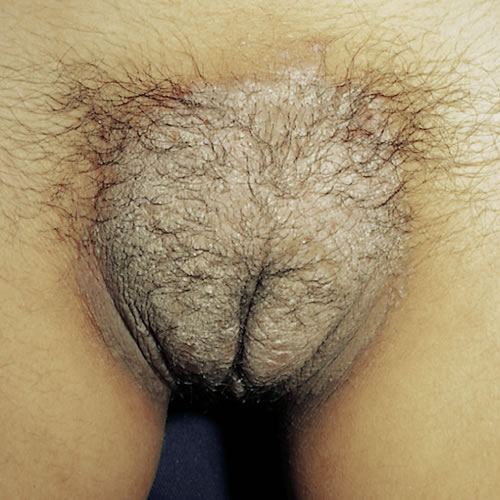
Scaling may not be present but psoriatic lesions are sharply demarcated. The inverse form occurs in a bilaterally symmetric pattern, with erythema, maceration, and fissuring extending in a linear fashion from the inguinal crease through the labiocrural fold and into the gluteal cleft.
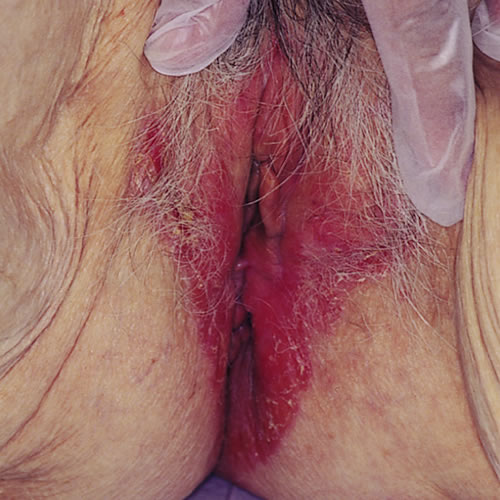
The gluteal cleft fissuring may be very difficult to manage. The mucosal area of the vulva is not involved except in the rare pustular form and in the lesions of Reiter’s disease. 9 Secondary changes such as excoriations, lichenification, crusting, and bacterial and yeast infections confuse the classic picture in many patients.
Psoriasis is not a scarring dermatosis, that is, there is typically no loss of normal anatomy related to psoriasis. However, some patients with psoriasis have loss of the labia minora.10 It is impossible in these patients to be certain that lichen sclerosus or lichen planus was not a pre-existing condition. Many patients with lichen sclerosus have psoriasis or have a first-degree relative with psoriasis. 11
Nail abnormalities include pitting, and brownish discoloration of the nail plate. In some cases, the nail can lift from its underlying surface. Psoriatic arthritis is limited to the minority of patients, ranging from minimal inflammation to severe deforming disease. 12
Diagnosis
Diagnosis is clinical and should include a family history. Biopsy is seldom needed. Check other parts of the patient’s body (scalp, ears, elbows, knees, nails for pitting, and so forth.) for typical psoriasis to confirm the diagnosis.
Pathology/Laboratory Findings
The typical histology shows parakeratosis, acanthosis with elongation of the rete ridges, and a reduced or absent granular layer, often with collections of neutrophils in the epidermis. There may also be papillary edema, and perivascular dermal inflammation. Unfortunately, flexural psoriasis does not always demonstrate these histological findings. 13
Differential Diagnosis
Differential diagnosis includes seborrheic dermatitis, intertrigo, monilial or dermatophyte infection, lichen simplex chronicus, and contact dermatitis.
Treatment/management
Non-Specific.
Patients need to be instructed to avoid trauma, including all irritating soaps, lotions, detergents, and synthetic clothing. To control the itch, patients can use ice or cold gel packs.
Cleansing should be gentle, without the use of a washcloth and with a product such as Cetaphil cleanser or Dove soap. If eczematous, recommend the patient use sitz baths or compresses once or twice a day. The area should be patted (not rubbed) dry.
An antihistamine, hydroxyzine or doxepin, 25 to 75 mg at bedtime, may be prescribed for the itch.
Specific.
For mild to moderate psoriasis:
- Gently cleanse daily.
- Desonide 0.05% ointment twice a day or 1% hydrocortisone in pramoxine cream applied topically twice daily x 2 to 3 weeks, then a milder topical prn.
For severe psoriasis:
- Clobetasol or halobetasol 0.05% ointment applied in a thin film topically twice a day x 2 weeks, once daily x 2 weeks, then Monday, Wednesday, Friday x 2 weeks.
- Alternate with low-potency topical steroid ointments and switch to intermittent low-potency preparations for long-term care.
- Calcipotriene (Dovonex) 50 μg/g ointment7 can be used as an alternate to topical steroids, twice a day x 3 to 6 weeks, or consider the calcipotriol in the morning and topical steroid at night time.
For marked thickness:
- Triamcinolone acetonide (Kenalog-10) diluted one part with two parts of normal saline for injection using a 30-gauge needle. The use of EMLA, a topical anesthetic cream applied in a thick film under plastic wrap for 15 to 20 minutes, makes this procedure almost painless. It can be repeated at 2 to 3 week intervals.
For concurrent secondary infection:
- To cover yeast and/or bacterial superinfection, it may be best to combine anti-yeast cream (that is, ketoconazole 2%) with an anti-bacterial (that is, mupirocin ointment). Use these with the topical steroids in stubborn cases.
For severe generalized psoriasis:
- Consult with a dermatologist to consider systemic therapy with retinoids, methotrexate, or even cyclosporine, subjects beyond this text.
References
- Fisher BK and Margesson LJ. Genital Skin Disorders: Diagnosis and Treatment. 1998, Mosby, Inc. 167-169.
- Wolff K, Johnson RA, eds. Fitzpatrick’s Color Atlas & Synopsis of Clinical Dermatology, sixth ed. New York, McGraw Hill Medical, 2009. 53.
- Smith RL, Warren RB, Griffiths CE, et al. Genetic susceptibility to psoriasis: an emerging picture. Genome Med. 2009; 22(1):72.
- Wolff K, Johnson RA, eds. Fitzpatrick’s Color Atlas & Synopsis of Clinical Dermatology, sixth ed. New York, McGraw Hill Medical, 2009. 53.
- Wolk K, Mallbris L, Larsson P, et al. Excessive body weight and smoking associates with a high risk of onset of plaque psoriasis. Acta Derma Venereol. 2009; 89:492-497.
- Dediol I, Buljian M. Buljian D, et al. Association of psoriasis and alcoholism: psychodermatological issue. Psychiatr Danub. 2009; 21:9-13.
- Nijstem T, Wallee M. Complexity of the association between psoriasis and comorbidities. J Invest Dermatol. 2009; 129:1601-1603.
- Makredes M, Robinson Jr D, Bala M, et al. The burden of autoimmune disease: a comparison of prevalence ratios in patients with psoriatic arthritis and psoriasis. J Am Acad Dermatol. 2009; 61:405-410.
- Neill SM, Lewis FM. Non-infective cutaneous conditions of the vulva. In: Neill SM, Lewis FM, eds, Ridley’s The Vulva, third ed. Oxford, England, 2009,110.
- Albert S, Neill S, Derrick EK, Calonje E. Psoriasis associated with vulval scarring. Clin and Experim Dermatol. 2004; 29:354-356.
- Eberz B, Berghold A, Regauer S. High prevalence of concomitant anogenital lischen sclerosus and extra-genital psoriasis in adult women. Obstet and Gynecol. 2008; 111:1143-1147.
- Edwards, L. Red plaques and patches. In:Edwards, L, Lynch PJ, eds. Genital Dermatology Atlas, second ed, Philadelphia, Wolters Kluwer/ Lippincott Williams & Wilkins, 2011:63-65.
- Neill SM, Lewis FM. Non-infective cutaneous conditions of the vulva. In: Neill SM, Lewis FM, eds, Ridley’s The Vulva, third ed. Oxford, England, 2009,110.