Introduction
Any injury to the skin that causes disruption of the melanocytes and basement membrane can result in depigmentation or hypomelanosis, which can be either temporary or permanent.
Epidemiology and etiology
The causes, as in post-inflammatory hyperpigmentation, are exogenous (e.g., ionizing radiation) or endogenous (e.g., discoid lupus erythematosus). The inflammation results in loss of melanocytes resulting from damage or destruction at the level of the basement membrane.
Symptoms and clinical features
While precipitants should be sought, the patient may have forgotten any history of a preceding process.
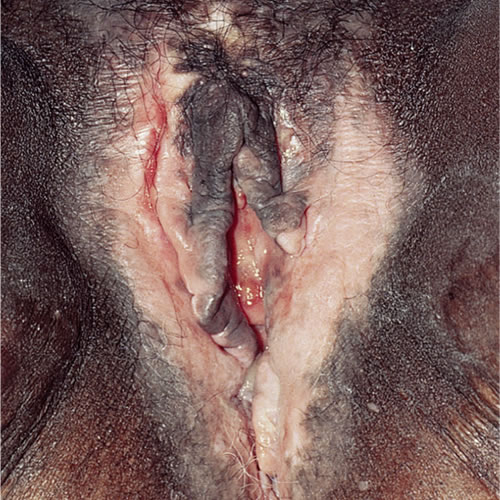
The skin color may be lightened (hypopigmented) or completely white (depigmented). The pattern on the vulva is variable, involving any portion, including the legs and thighs. It follows the shape of the original eruption and is much more noticeable in darker skin.
Pathology/Laboratory Findings
Melanocytes may still be found in tissue samples, but there is a decrease in the amount of melanin.
Diagnosis
Diagnosis is clinical, based on pattern and, if necessary, histopathology.
Differential diagnosis
Differential diagnosis includes vitiligo and lichen sclerosus.
Treatment
No therapy is necessary. Treating the underlying cause, if it is still active, hastens resolution and the pigmentation often returns with time. Reassure the patient the condition is completely harmless.