Introduction
Post-inflammatory hyperpigmentation refers to the end stage of a prior inflammatory process that deposits melanin in the dermis but gives no clues as to the nature of the original problem.
Epidemiology and etiology
Pigmented macules or patches can be seen on the skin after any inflammatory injury.1 Exogenous causes include physical or chemical agents used either topically or internally. Topical examples include soaps, cleansers, and topical allergens; internal causes are usually drugs (fixed drug eruption). Endogenous causes of inflammation include lichen planus,, lichen sclerosus, discoid lupus erythematosus, and psoriasis. In either case, there is an increase in production of melanosomes.2
Symptoms and clinical features
The patient gives a history of a preexisting inflammatory process or injury, although sometimes the history may be missed (e.g., in a fixed drug eruption when the patient noted little or no prior inflammation).
Varying degrees of macular or patchy hyper-pigmentation occur. The color can be brown to black, is usually irregular, and can show scattered patches of hypo-pigmentation.
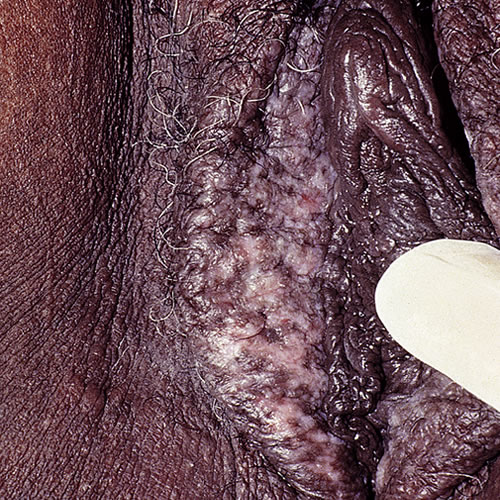
The pigment intensity depends on the severity of the original inflammation and the natural background pigmentation.
Diagnosis
Clinical picture and histopathology determine the diagnosis.
Pathology/Laboratory Findings
Because of the difficulty in distinguishing benign hyperpigmentation from pre-cancer or melanoma, the clinician will often need to biopsy hyperpigmented tissue.
Differential diagnoses
The differential includes benign vulvar melanosis and vulvar intraepithelial neoplasia.
Treatment
No treatment is needed for this condition. Any inflammatory process that is ongoing should be treated. With time, the pigmentation should fade.
References
- Fisher BK and Margesson LJ. Genital Skin Disorders: Diagnosis and Treatment. 1998. Mosby. 188.
- Stulberg DL, Clark N. Common hyperpigmentation disorders in adults. Part 1. Diagnostic approach, café au lait macules, diffuse hyperpigmentation, sun exposure, phototoxic reactions. Am Fam Physician. 2003; 68(10): 1955-1960.