Erosive lichen planus of the vagina is covered in Annotation O: The vaginal epithelium
Introduction
Lichen planus presents as a papulosquamous skin eruption with or without mucous membrane involvement. It can involve an array of tissue, including, but not limited to, oral mucosa, the vulva, vagina, anus, and esophagus, as well as the scalp and nails. The oral mucosa is the most common site involved and 25-57% of women with oral LP will have vulvovaginal involvement.1
Synonyms for vulvovaginal lichen planus are erosive vaginal lichen planus, vulvovaginal-gingival syndrome, ulcerative lichen planus, and LP. There is controversy over whether desquamative inflammatory vaginitis and vaginal lichen planus are the same entity.
Epidemiology
Lichen planus is associated with vulvar disease more commonly than previously suggested, usually involving patients 50 to 60 years old (age range 29-82). The estimated incidence among the general population is 1-2%.2
Etiology
The cause of lichen planus is unknown. It is probably an autoimmune disorder at the cellular level.3 4 One theory suggests that the condition is T-cell mediated, resulting in destruction of basal keratinocytes. The responsible antigen is unknown.5
Some drugs induce lichen planus-like (lichenoid) eruptions anywhere on the body, including in the vulvar area. These include beta blockers, hydrochlorothiazide, methyldopa, penicillamine, quinidine, non-steroidal anti-inflammatories (NSAIDs), angiotenein converting enzyme (ACE) inhibitors, sulfonylurea agents, carbamezepine, gold, lithium, and quinine.6 Drugs most frequently involved in induction or worsening of LP are hydrochlorothiazide and nonsteroidal anti-inflammatory drugs (NSAIDs).7 A trial of three to four weeks off a questionable drug may result in clearance or significant improvement, aiding diagnosis.
Symptoms and clinical features
The disease occurs in three patterns:
- The classic papulosquamous form presents with the five Ps — pruritic, purple, polyhedral papules, and plaques — and classically involves the wrists and ankles. The vulvar involvement is part of a generalized disease with the papules and plaques on the labia majora, thighs, and mons pubis. There is no atrophy or scarring. The trauma of scratching spreads the papules, a phenomenon termed Koebnerization. There is a history of severe itching in the papulosquamous form, but limited involvement in the vulvar area. The patient may be unaware of involvement in either the mouth or vulvar area. Both areas should always be checked. This form is rare, and often patients are asymptomatic; when symptomatic they are highly responsive to standard treatment.8
- The erosive form, encompassing vulvovaginal gingival syndrome is a destructive form of lichen planus involving the non-keratinized skin such as the mucous membranes of the mouth and vulvovaginal area (vestibule, labia minora, and vagina), with atrophy and scarring. 9 This is the most common variant of the three 10 In this form, pain, burning, and irritation occur and may be responsible for severe dyspareunia and dysuria. Itching is somewhat less common and scratching is not soothing. Extensive vaginal involvement may result in a purulent, malodorous discharge. The associated dyspareunia leads to depression, anger, frustration, and relationship distress. There may initially be no erosions, just simply tiny white 1 mm papules, often in a linear, fernlike, or lacy reticular pattern on the buccal mucosa or along the edges of the vulvar trigone. The degree of erosion is variable in either site. Close and regular follow up with a dental specialist comfortable with lichen planus is important given potential for malignancy.11 In extensive disease, the whole vulvar trigone and vaginal area may be denuded and open with a weeping discharge. Over time there is scarring with loss of normal anatomy, affecting the clitoris and labia minora, with vaginal adhesions. Ultimately, there is gradual but progressive destruction of the vagina. This form is chronic, very destructive, debilitating, and difficult to treat. Desquamative inflammatory vaginitis (DIV) is an intensely inflammatory vaginitis, also called lichenoid vaginitis, thought to be associated with lichen planus in some instances. Women present with a purulent vaginal discharge which has an elevated pH, sheets of white blood cells and preponderance of parabasal cells on saline wet prep, indicative of desquamating vaginal epithelium. There is bacterial overgrowth, except for lactobacillus, which is absent.
- The hypertrophic is the least common form. It presents with extensive white scarring of the periclitoral area extending along the interlabial sulcus to the introitus with variable degrees of hyperkeratosis. It looks like lichen sclerosus but is treatment resistant. This form may be very itchy. Dyspareunia is a problem when there is scarring. When chronic, there is burying of the clitoris, loss of labia minora, and introital stenosis. At times it can be difficult to distinguish from malignancy and therefore there should be a low threshold to biopsy.12
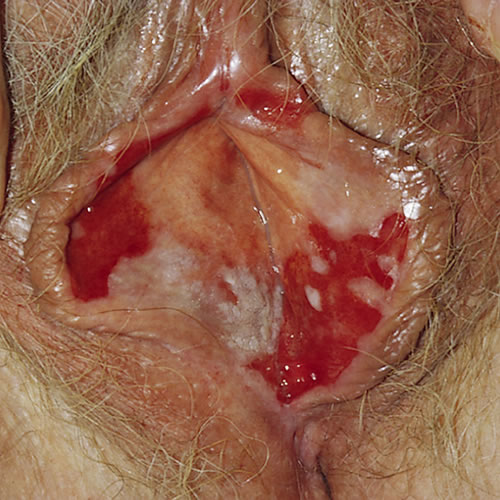
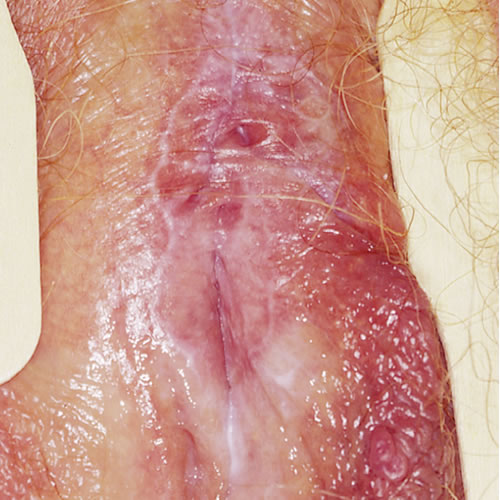 In extensive disease, the whole vulvar trigone and vaginal area may be denuded and open with a weeping discharge.
In extensive disease, the whole vulvar trigone and vaginal area may be denuded and open with a weeping discharge.
Diagnosis
Diagnosis of lichen planus is often delayed and at times clinically difficult to make, even with assistance of a biopsy, given the high incidence of inconclusive histopathology seen in 30-40% of biopsies.13 There is no defined set of criteria for diagnosing erosive lichen planus affecting the vulva (ELPV) and there is geographical variation in management. A three-stage international electronic-Delphi exercise with a subsequent formal feedback process achieved consensus for the following ‘supportive’ diagnostic criteria:
Consensus Delphi committee-recommended clinical and histological characteristics of erosive lichen planus14
| 1. Well-demarcated erosions/erythematous areas at the vaginal introitus |
| 2. Presence of a hyperkeratotic border to lesions and/or Wickham striae in surrounding skin |
| 3. Symptoms of pain/burning |
| 4. Scarring/loss of normal architecture |
| 5. Presence of vaginal inflammation |
| 6. Involvement of other mucosal surfaces |
| 7. Presence of a well-defined inflammatory band involving the dermo-epidermal junction |
| 8. Presence of an inflammatory band consisting predominantly of lymphocytes |
| 9. Signs of basal layer degeneration on biopsy |
It was suggested that at least three supportive features should be present to make a diagnosis of ELPV, although this number is subject to further discussion.15
In 2020, the ISSVD tasked the Difficult Pathologic Diagnoses committee with the development of diagnostic criteria based on literature review of available LP studies since 1990, producing the following recommended criteria:
Recommended clinical and histological criteria for erosive lichen planus from the ISSVD Difficult Pathologic Diagnoses Committee, 202016
|
1. Well-demarcated, glazed red macule or patch at labia minora, vestibule, and/or vagina |
|
2. Disease affects hairless skin, mucocutaneous junction, and/or nonkeratinized squamous epithelium |
|
3. Evidence of basal layer damage, categorized as degenerative or regenerative |
|
4. A closely applied band-like lymphocytic infiltrate |
|
5. Absent subepithelial sclerosus |
For the papular form and non-erosive disease, the clinical diagnosis can be confirmed by biopsy. In extensive erosive disease, once familiar with the visual pattern, the clinician may make the diagnosis based on the exam alone. Biopsy may help but is not always confirmatory; some studies report that only 71% of biopsies are diagnostic.17. When done, biopsies should be taken at the edge of the skin of interest, including normal and abnormal skin to aid in diagnosis. 18 Demonstration of typical oral changes carries more diagnostic weight than biopsy.
A lichenoid drug eruption can be indistinguishable clinically and histologically from lichen planus.19 History of taking a particular medication and improvement of skin lesions after stopping the drug will make this diagnosis more likely.
Malignancy potential
A slightly increased risk of vulvar malignancy in women with vulvar lichen planus was reported, but not confirmed in large series.20 A search of MEDLINE, EMBASE, and Cochrane Library databases combined findings from four case series to show that vulvar squamous cell carcinoma (VSCC) occurred in 5 of 366 patients. Insufficient data are present from the identified case series to calculate the incidence and prevalence of VSCC within the population with ELPV.21
There is clear evidence that the risk of malignancy associated with lichen sclerosus appears to be 4-5%. Although there is a suggestion of an increased prevalence of VSCC in patients with ELPV, the only way to clarify this is for long-term follow-up data of the disease and its complications to be recorded in a multi-center registry. Additionally, a study in Austria that included 38 women suggested that VSCC in patients with lichen planus had a worse prognosis and was more aggressive, further stressing the need to look into this possible correlation.22
Pathology/Laboratory Findings
Hypertrophic lichen planus: “Typical changes are irregular acanthosis with a saw-tooth appearance of the rete pegs, an increased granular layer, and disruption of the basal layer with a closely apposed dermal band-like lymphocytic infiltrate. The acanthosis and hyperkeratosis are marked in the hypertrophic form and because of the chronicity of this form the characteristic band-like infiltrate is not obvious but will be found focally. Eosinophilic colloid bodies may be seen. Immunoflurorescent (IMF) studies will reveal uneven fibrinogen staining of the basement membrane and IgM cytoid bodies.”23
Classic lichen planus: “The stratum corneum shows hyperkeratosis and the granular cell layer displays homogenous or wedge-shaped hypergranulosis” and the “prickle cell layer is acanthotic, often with spiky rete ridges. The basal layer has vacuolar change, apoptotic bodies, and/or squamatization, as well as lymphocytosis. The dermis contains a closely applied band-like lymphocytic infiltrate that also has may have histiocytes, plasma cells, and occasional neutrophils and eosinophils.”24
Erosive lichen planus: Classical findings on biopsy specimens are a dense, lymphocytic, dermal bandlike infiltrate extending to and causing disruption of the basal layer.
The three histological findings common between all three sub-types are: basal layer damage, lymphocytic infiltrate, absent sclerosus.25
Differential diagnosis
Differential diagnoses of the papulosquamous form include psoriasis, dermatophyte infection, lichen simplex chronicus and lichen sclerosus. It is helpful to remember that lichen sclerosus does not affect the vagina.
For erosive disease, the differential diagnoses include lichen sclerosus, plasma cell vulvitis, cicatricial pemphigoid, pemphigus, lupus erythematosus and bullous pemphigoid.
Additionally, it is not rare to have both lichen planus and sclerosus, therefore multiple biopsies should be considered in grossly different skin, especially given the difference in malignant potential between the two.26
Treatment/management
Treatment requires the expertise of a dermatologist or knowledgeable gynecologist. Erosive lichen planus is extremely difficult to treat; no single effective therapy exists at this time. By comparison, hypertrophic and papulosquamous lichen planus respond well to therapy. Treatments are listed in order of preference.
1. Papulosquamous and hypertrophic lichen planus: Aim to manage the itching and the scratching. (see General Therapy below.) A two week course of a moderate or superpotent topical glucocorticoid (as described below), usually results in complete remission or significant improvement of the disease. Intralesional steroids (20 mg/mL triamcinolone may be needed). Oral retinoids may be very helpful.
2. Oral lichen planus: A relatively effective treatment27 is achieved through the use of a topical ultrapotent glucocorticoid gel or ointment such as Clobetasol 0.05% applied daily for six months. In one study, antimycotic treatment consisting of miconazole gel and 0.12% chlorhexidine mouthwashes enhanced treatment.28
3. Erosive lichen planus of the vulva: First line treatments are topical ultrapotent glucocorticoids used daily initially and then weekly for maintenance once symptoms are improved. Flares need to be managed with return to more frequent use of the topical steroids temporarily. All women with this chronic disease need to be educated about it. Handout on lichen planus. They will need to continue treatment even after symptoms have improved. They need emotional support and reassurance that the condition is manageable, despite dyspareunia and anatomical changes.
General therapy
- Avoidance of irritants: including scented soaps or shampoos, feminine sprays, douches, powders or wipes, sanitary napkins or daily panty liners, tight clothing (including lycra) or panty hose, lengthy hot baths, rough washcloths, hair dryers to the vulva, etc.
Rather, advise cool, loose, ventilated clothing (cotton may be best), fragrance-free, pH neutral soaps (Dove or Basis unscented soap or Cetaphil cleanser,) finger-tip washing, short, warm water soaks and patting dry gently. - Hydration of the skin: Warm water soaks for five to ten minutes in a tub or sitz bath can be very soothing to the skin, rehydrating sore, dry or cracked tissue and opening the pores to allow better penetration of medication. Topical application of an emollient after gentle drying will help to maintain the benefits of hydration. White petrolatum is recommended.
- Reduction of itching: Educate that itching can be caused by pressure and friction from tight clothing, drying of the skin from overwashing, the use of topical cleansing or deodorizing products, menstrual products, exercise gear, secretions and sweat, synthetic fabrics, chemicals in detergents, fabric softeners and bleaches, as well as by overt allergic reaction or skin disease or infections, including but not limited to yeast. Itching causes scratching which can produce further itching, as well as break down of the skin. It is very important to remove this symptom to promote healing. Treatment of the precipitating condition is the first priority, but women sometimes need more support to reduce itching.
Application of topical numbing agents such as Lidocaine 5% ointment can reduce the impulse to scratch. Warn patients that Lidocaine may burn for up to 45 seconds before numbing the skin.
Application of cold gel packs can be very soothing.
Night-time scratching can be controlled with a sedative antihistamine taken at bedtime, such as a small oral dose (10 mg) of Atarax. These drugs work against the itch-producing chemical histamine and also cause sleepiness.29 - Stop oral medications that might be causing a reaction in the skin: Some drugs that are associated with lichenoid reactions are: beta-blockers, methyldopa, penicillamine, quinidine, nonsteroidal anti-inflammatory drugs (NSAIDs), angiotensin converting enzyme (ACE) inhibitors, sulfonylurea agents, carbamazepine, gold, lithium, and hydrochlorothiazide.30 Other drugs have been reported in isolated case reports. Hydrochlorothiazide and NSAIDs are common triggers for lichen planus; a three-week trial off these medications will show whether discontinuation is likely to improve symptoms.
Specific Treatment
First-line medical treatment for erosive vulvar lichen planus consists of ultrapotent topical glucocorticoids which will give relief of symptoms in 71% of patients. With time and treatment, three quarters can expect overall improvement of symptoms and one half, healing of erosions.31
Other studies have shown up to 94% symptomatic improvement and 71% of patients symptom free with regular use of topical ultrapotent steroids.32. Non-erosive disease can be treated with mid or low potency topical steroids.33
- Improper application of the topical medication is a common reason for treatment failure. We use a mirror to show the patient the areas of the vulva affected by the disease so she will apply her topical medications appropriately; diagrams and descriptions alone are inadequate, especially in the elderly. We also emphasize that the amount of topical glucocorticoid used should be the size of a 2 to 3 mm dot. During the first week of therapy, a five-minute sitz bath in water at a comfortable temperature (followed by gentle drying with a soft towel) hydrates the skin, making it more receptive to the medication.
- Topical Steroids:
- Clobetasol 0.05%, halobetasol 0.05% or betamethasone dipropionate 0.05% ointment in an augmented vehicle: Apply in a thin film twice a day for 30 days for severe disease, then reduce the frequency to once a day for 30 days, then two or three times a week for a total of 12 weeks.
- An ointment is the preferred formula given as it is better absorbed, serves as an emollient, and is less likely to have preservatives that can cause an irritant dermatitis.34
- For less severe disease, application nightly for the first 30 days and then reduction down to two or three times a week for 12 weeks may be sufficient. The lowest frequency that controls symptoms is prescribed.35 The patient is re-evaluated in one to three months depending on the severity
- If the medication is completely discontinued at this point, symptoms of lichen planus will return; therefore, after the initial 12-week course of treatment, we begin maintenance therapy with a midpotency (e.g. betamethasone valerate 0.1%) or a low potency glucocorticoid ointment (e.g. 2.5 percent hydrocortisone ointment) one to three times per week indefinitely; “trial and error” is necessary to find the lowest dose and frequency that control symptoms.36 Consultation with a dermatologist is helpful for managing topical glucocorticoids.
- If relapse occurs after initial benefit during the initial 12 weeks of therapy or during the maintenance phase, we restart an ultrapotent glucocorticoid nightly for a month, then taper to every other night for a month, then taper to three times per week maintenance therapy.
- Intramuscular triamcinolone: For patients with erosive disease that is too severe on initial presentation to allow application of topical clobetasol or halobetasol, we administer one dose of triamcinolone (1 mg/kg, intramuscularly) and then begin superpotent topical therapy two weeks later. Protecting the vulva by application of petroleum jelly during the two-week interval helps the epithelium to replace cells lost to erosion.
Intralesional triamcinolone: 3.3-10 mg/mL (Kenalog-10) diluted 1:2 with saline and repeated every 3-4 weeks x 3 using a 30-gauge needle; high doses should not be given in a small area as erosions and ulcers may occur. - Systemic corticosteroids: Prednisone 40-60 mg orally a day can ameliorate symptoms in most patients but symptoms recur on stopping the medication. This is not a first-line medication in this case and should be used in combination with topical steroids.37
- Topical calcineurin inhibitors are non-steroidal immunomodulatory medications now often used in the treatment of skin disease. If there is no improvement with glucocorticoids, our second-line therapy is tacrolimus. Results from small case series suggest that topical tacrolimus can be effective for treatment of vulvovaginal (and oral) lichen planus,38 39 40 41 though improvement can be delayed in comparison to topical steroids42 In a small retrospective study of patients unresponsive to topical steroids, 94% of patients responded to topical tacrolimus with regular daily use44 We continue therapy for up to 12 weeks as long as there is continue improvement in symptoms, then reduce the dose to maintenance therapy: one to three times weekly, as needed to control symptoms.45 Monitoring drug levels is unnecessary with topical therapy. Of note, tacrolimus carries a black box warning for increased risk of squamous cell carcinoma. However, to date, there is no strong evidence of cancer associated with topically applied tacrolimus. Pimecrolimus works similarly, however, is more selective regarding target cells and therefore side effects are reportedly more tolerable in comparison to tacrolimus.46
- Other systemic treatment: Data regarding systemic therapy is limited and the majority involve small case studies and no controlled trials.47 Furthermore, response to systemic treatments other than oral or IM steroids often takes longer and a minimum trial of 3 months is recommended prior to discontinuation and switching to another treatment.48 One such systemic treatment includes oral methotrexate at doses between 2.5 and 15 mg weekly in combination with topical treatment (most often an ultrapotent steroid or tacrolimus).49, 50 A retrospective study of 27 patients at Wake Forest Baptist Hospital demonstrated 19 patients (70%) with improvement including 14 patients (52%) with improvement at 1 month follow up.51 The most commonly reported side effects were fatigue and gastrointestinal distress.52
- Adalimumab, azathioprine, cyclosporine, and mycophenolate mofetil have also been used in small studies, but with even smaller data regarding effectiveness and side effect profile.53 Acitretin and isotretinoin, systemic retinoids, have shown some benefit for unresponsive hypertrophic disease.54 However, these medications are teratogenic and therefore should be used with caution in women of reproductive age.55 Oral cyclosporine demonstrated benefit among 5 patients over 3 months.56 Hydroxychloroquine 200 mg twice daily is another low cost option with minimal laboratory monitoring required.57 58 Though few studies have assessed the efficacy of myocophenolate mofetil, they have all consistently demonstrated a more favorable side effect profile in comparison to other systemic medications.59
- Topical Estrogen: In postmenopausal women, topical estrogen can help to make thinning skin more supple and resilient, supporting treatment. It can also be beneficial in the vaginal environment. The combination of topical estrogen and steroid ointments, however, can make women more susceptible to yeast infections.
- Other: Some patients have found topical aloe vera to be beneficial, likely due to its anti-inflammatory benefits, but available studies are quite small and additional investigation is needed.60 Topical photodynamic therapy (PDT) is another treatment currently under investigation given benefit seen in oral lichen planus, but again needing larger studies to support its role in vulvovaginal LP.61 Furthermore, PDT is painful, and in a prior RCT, required general sedation during treatment. Significant pain relief up till one year after one treatment and renewed need for topical steroids were reported by the patients.62
- Treatment of concurrent infection: An associated bacterial or fungal infection should be treated concurrently with glucocorticoid therapy. Antibiotic selection should be based upon culture and sensitivity results. Erythromycin 250 mg orally four times a day for 5 to 7 days or a cephalosporin, e.g. cephalexin 500 mg orally three times a day for 5 to 7 days covers most bacterial infections. We give the patient oral fluconazole (150 mg by mouth every other day for three doses, then 150 mg weekly for three weeks) to avoid or treat concomitant candidiasis.
- Topical Steroids:
Pain control
Acetaminophen plus codeine
Special Situations:
Vaginal stricture: Annotation O Is the vaginal epithelium normal?
Emotional Support: These patients need help and understanding. They must be involved, along with their partner, in psychosexual counseling for this difficult and chronic condition. Multiple studies have reported sexual distress, moderate effect on quality of life, dyspareunia, and several years of sexual abstinence as a result of their diagnosis.63 Realistic expectations must be defined to avoid disappointment with therapy and dissatisfaction with the therapists.
We also work with pelvic floor physical therapists if the patient would like to be sexually active but has pelvic floor hypertonicity.
References
- Day T, Wilkinson E, Rowan D, Scurry J; ISSVD Difficult Pathologic Diagnoses Committee. Clinicopathologic Diagnostic Criteria for Vulvar Lichen Planus. J Low Genit Tract Dis. 2020 Jul;24(3):317-329. doi: 10.1097/LGT.0000000000000532. PMID: 32205763.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Astralas J Dermatol 2019 Feb;60 (1):7-11. Doi 10.111/ajd. 12875. Epub 2018 Jul 1. PMID : 29961956.
- Lehman JS, Tollefson MM, Gibson LE. Lichen planus. Int J Dermatol. 2009;48(7):682.
- Sontheimer RD, Lichenoid tissue reaction/interface clinical and histological perspectives. J Invest Dermatol. 2009;129: 1088-1099.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb:60(1):7-11.
- Thompson DF, Skaehill PA. Drug-induced lichen planus. Pharmacotherapy. 1994;14(5):561.
- Gunes AT, Fetil E, Ilknur T, et al. Naproxen-induced lichen planus: report of 55 cases. Int J Dermatol. 2006:45:709.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Day T, Weigner J, Scurry J. Classic and Hypertrophic Vulvar Lichen Planus. J Low Genit Tract Dis. 2018 Oct;22(4):387-395. doi: 10.1097/LGT.0000000000000419. PMID: 29994816; PMCID: PMC6296835.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Wu M, Lee G, Fischer G. Forming diagnostic criteria for vulvar lichen planus. Australas J Dermatol. 2020 Nov;61(4):324-329. doi: 10.1111/ajd.13350. Epub 2020 Jul 16. PMID: 32671833.
- Simpson R, Thomas K, Leighton P, Murphy R. Diagnostic criteria for erosive lichen planus affecting the vulva: An International electronic-Delphi consensus exercise. Br J Dermatol. 2013; 169(2):337-43.
- Simpson R, Thomas K, Leighton P, Murphy R. Diagnostic criteria for erosive lichen planus affecting the vulva: An International electronic-Delphi consensus exercise.Br J Dermatol. 2013; 169(2):337-43.
- Day T, Wilkinson E, Rowan D, Scurry J; ISSVD Difficult Pathologic Diagnoses Committee. Clinicopathologic Diagnostic Criteria for Vulvar Lichen Planus. J Low Genit Tract Dis. 2020 Jul;24(3):317-329. doi: 10.1097/LGT.0000000000000532. PMID: 32205763.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focussed review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focused review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Ridley CM, Neill SM. Genital Dermatology, Libby Edwards, ed. Lippincott Williams and Wilkins, Philadelphia 2004. P 14.
- Kennedy CM, Peterson LB, Galask RP. Erosive vulvar lichen planus: a cohort at risk for cancer? J Reprod Med. 2008; 53:781.
- Simpson R, Murphy R. Is vulvar erosive lichen planus a premalignant condition? Arch Dermal 2012; 148(11):1314-16.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Heller DS, Wallach RC: Vulvar Disease: A Clinicalpathological Approach, Informa Healthcare, 2007. 42-43.
- Day T, Wilkinson E, Rowan D, Scurry J; ISSVD Difficult Pathologic Diagnoses Committee. Clinicopathologic Diagnostic Criteria for Vulvar Lichen Planus. J Low Genit Tract Dis. 2020 Jul;24(3):317-329. doi: 10.1097/LGT.0000000000000532. PMID: 32205763.
- Day T, Wilkinson E, Rowan D, Scurry J; ISSVD Difficult Pathologic Diagnoses Committee. Clinicopathologic Diagnostic Criteria for Vulvar Lichen Planus. J Low Genit Tract Dis. 2020 Jul;24(3):317-329. doi: 10.1097/LGT.0000000000000532. PMID: 32205763.
- Day T, Moore S, Bohl TG, Scurry J. Comorbid Vulvar Lichen Planus and Lichen Sclerosus. J Low Genit Tract Dis. 2017 Jul;21(3):204-208. doi: 10.1097/LGT.0000000000000307. PMID: 28369011.
- Carbone M, Conrotto D, Carrozzo M, Broccoletti R, Gandolfo S, Scully C. Topical corticosteroids in association with miconazole and chlorhexidine in the long-term management of atrophic-erosive oral lichen planus: a placebo-controlled and comparative study between clobetasol and fluocinonide. Oral Dis. 1999;5(1):44.
- Carbone M, Conrotto D, Carrozzo M, Broccoletti R, Gandolfo S, Scully C. Topical corticosteroids in association with miconazole and chlorhexidine in the long-term management of atrophic-erosive oral lichen planus: a placebo-controlled and comparative study between clobetasol and fluocinonide. Oral Dis. 1999;5(1):44.
- Stewart EG, Spencer P. The V Book: a doctor’s guide to complete vulvovaginal health. Bantam Books, 2002. 261.
- Ball SB, Wojnarowska F. Vulvar dermatoses: lichen sclerosus, lichen planus, and vulval dermatitis/lichen simplex chronicus. Semin Cutan Med Surg. 1998; 17:182.
- Cooper Sm, Wojnarowska F. Influence of treatment of erosive lichen planus of the vulva on its prognosis. Arch Dermatol. 2006; 142:289.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focussed review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Cooper Sm, Wojnarowska F. Influence of treatment of erosive lichen planus of the vulva on its prognosis. Arch Dermatol. 2006; 142:289.
- Ridley CM, Neill SM. Non-infective cutaneous conditions of the vulva. In: The Vulva. Ridley CM, Neill SM, eds. Blackwell Science, Oxford 1999. 121.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Kennedy CM, Galask RP. Erosive lichen planus: retrospective review of characteristics and outcomes in 113 patients seen in a vulvar specialty clinic. J Reprod Med. 2007; 52:43.
- Kirtschig G, Van Der Meulen AJ, Ion Lipan JW, Stoof TJ. Successful treatment of erosive lichen planus with topical tacrolimus. Br J Dermatol. 2002; 147:625.
- Byrd JA, Davis MD, Rogers RS 3rd. Recalcitrant symptomatic vulvar lichen planus: response to topical tacrolimus. Arch Dermatol. 2004; 140:715.
- Jensen JT, Bird M, Leclair CM. Patient satisfaction after the treatment of vulvovaginal erosive lichen planus with topical clobetasol and tacrolimus: a survey study. Am J Obstet Gynecol. 2004; 190: 1759.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.[/efn_note ]Patients are warned that 30-50% of women who try tacrolimus have vulvar burning initially. In some cases, burning may disappear within a few days of use. We prescribe 0.03% or 0.1 % ointment. The patient should apply the smallest amount needed to coat the lesion in order to minimize burning and irritation, and then rub it in well. We begin with every other day treatments, gradually working up to twice daily. Daily sitz baths for the first week of therapy can help alleviate burning. To minimize burning, tacrolimus can be applied on top of the glucocorticoid ointment or on top of a coat of petroleum jelly. Jacques et al. report anecdotal experience of greater symptom reduction and response among patients who did experience burning.43Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Jensen JT, Bird M, Leclair CM. Patient satisfaction after the treatment of vulvovaginal erosive lichen planus with topical clobetasol and tacrolimus: a survey study. Am J Obstet Gynecol. 2004; 190: 1759.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focussed review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focussed review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Cline A, Cuellar-Barboza A, Jorizzo JL, Pichardo RO. Methotrexate for the Treatment of Recalcitrant Erosive Lichen Planus of the Vulva. JAMA Dermatol. 2020 Feb 1;156(2):215-217. doi: 10.1001/jamadermatol.2019.4062. PMID: 31895434; PMCID: PMC6990954.
- Cline A, Cuellar-Barboza A, Jorizzo JL, Pichardo RO. Methotrexate for the Treatment of Recalcitrant Erosive Lichen Planus of the Vulva. JAMA Dermatol. 2020 Feb 1;156(2):215-217. doi: 10.1001/jamadermatol.2019.4062. PMID: 31895434; PMCID: PMC6990954.
- Dubey R, Fischer G. Vulvo-vaginal lichen planus: A focussed review for the clinician. Australas J Dermatol. 2019 Feb;60(1):7-11. doi: 10.1111/ajd.12875. Epub 2018 Jul 1. PMID: 29961956.
- Schlosser BJ, Mirowski GW. Lichen sclerosus and lichen planus in women and girls. Clin Obstet Gynecol. 2015 Mar;58(1):125-42. doi: 10.1097/GRF.0000000000000090. PMID: 25608255.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Schlosser BJ, Mirowski GW. Lichen sclerosus and lichen planus in women and girls. Clin Obstet Gynecol. 2015 Mar;58(1):125-42. doi: 10.1097/GRF.0000000000000090. PMID: 25608255.
- Edwards L, and Lynch P. Genital Dermatology Atlas and Manual, 3rd Edition. Wolters Kluwer 2018.
- Mauskar MM, Marathe K, Venkatesan A, Schlosser BJ, Edwards L. Vulvar diseases: Conditions in adults and children. J Am Acad Dermatol. 2020 Jun;82(6):1287-1298. doi: 10.1016/j.jaad.2019.10.077. Epub 2019 Nov 8. PMID: 31712170.
- Deen K, McMeniman E. Mycophenolate mofetil in erosive genital lichen planus: a case and review of the literature. J Dermatol. 2015 Mar;42(3):311-4. doi: 10.1111/1346-8138.12763. Epub 2015 Jan 13. PMID: 25583369.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.
- Helgesen AL, Warloe T, Pripp AH, Kirschner R, Peng Q, Tanbo T, Gjersvik P. Vulvovaginal photodynamic therapy vs. topical corticosteroids in genital erosive lichen planus: a randomized controlled trial. Br J Dermatol. 2015 Nov;173(5):1156-62. doi: 10.1111/bjd.14033. Epub 2015 Oct 16. PMID: 26189484.
- Jacques L, Kornik R, Bennett DD, Eschenbach DA. Diagnosis and Management of Vulvovaginal Lichen Planus. Obstet Gynecol Surv. 2020 Oct;75(10):624-635. doi: 10.1097/OGX.0000000000000834. PMID: 33111963.