Introduction
Benign familial pemphigus1 is a rare, superficial, blistering disease of the intertriginous areas—usually the groin and axillae.
Synonyms for benign familial pemphigus are Hailey-Hailey disease (the name giving credit to the two brothers who first described it in 1939) and benign familial chronic pemphigus.
Epidemiology
The onset usually occurs early in adult life, during the second or third decade, but may be delayed until the fourth or fifth decade.2 The prevalence is unknown and there is no known predilection for race or gender.
Etiology
The multifactorial etiology includes an autosomal dominant predisposition to which the addition of minor friction, heat, dampness, and superimposed infection results in loss of keratinocyte cohesiveness with subsequent formation of small blisters and erosions. Spontaneous occurrence with no past family history is possible.
The defect responsible has now been identified on a gene called ATP2C1 found on chromosome 3q21-24.3 This gene codes for the protein SPCA1 (Secretory Pathway Calcium/manganese-ATPase), a calcium and manganese pump. The skin cells (keratinocytes) adhere via structures called desmosomes and it seems the desmosomes do not assemble properly if there is insufficient calcium. Normally, the cells are packed together tightly similar to bricks and mortar. Patients with Hailey-Hailey disease have defective ‘mortar’ and the cells fall apart, like a crumbling brick wall.
There is no known cure.
Symptoms and clinical features
In an environment of heat, sweating, and friction, patients complain of burning, soreness, and irritation in the axillae and groin. Hailey-Hailey disease is associated with colonization and secondary bacterial, viral, and fungal infections.
In the axillae and groin, annular and serpiginous groups of vesicles rupture and leave a rim of scaling and yellowish crusting and erosions. As these annular plaques extend, the central skin appears fissured and cracked and there may be a fair amount of maceration. Typically, this is in the folds of the axillae. In the genital area, the inguinal crease is involved, with the lesions extending down along the edge of the labia majora and out onto the thighs.
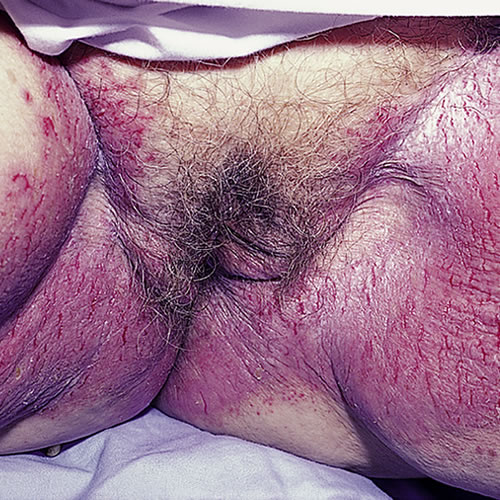
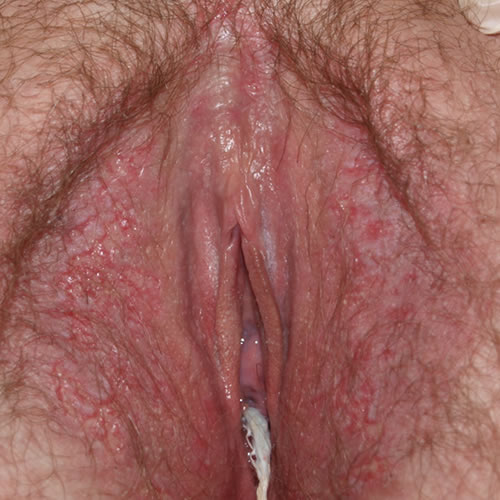
Irritated areas can appear as short, irregular, linear fissures. There can also be involvement around the neck, trunk, and under the breasts. Bacteria or yeast superinfection is common, producing an unpleasant odor. This condition does not affect mucosa.
Diagnosis
Diagnosis is based on the clinical picture and histopathology. The absence of oral lesions separates this condition from the other forms of pemphigus.
Pathology/Laboratory Findings
Biopsy is helpful in making the diagnosis.
Differential diagnosis
Differential diagnoses include intertrigo, Candidiasis, herpes simplex virus infections, tinea cruris, secondarily infected eczema or inverse psoriasis, and pemphigus.
Treatment/management
This requires a dermatologist. Management is aimed at symptom control and treatment of secondary infection because there is no true satisfactory treatment. These patients have flare-ups whenever they are in an environment of excess heat, moisture, and friction.
General
Treatment is aimed at controlling the local environment and minimizing secondary superinfection. Recommendations to the patient include weight loss, avoidance of over-heating, and the use of loose ventilated clothing with layers of thin cotton fabric between the skin folds to decrease moisture and friction.
A topical antibiotic cream (e.g., clindamycin or erythromycin) and an anticandidal cream (e.g., 2% miconazole) can be used together in a thin film twice a day with a light dusting (not enough to cause caking) of absorbent powder (Zeasorb). For secondary bacterial infections, appropriate systemic antibiotics may be necessary after the culture and sensitivity are obtained.
Specific
A mild topical corticosteroid, such as hydrocortisone acetate 2.5% cream twice a day, can be useful for inflammation. Topical cyclosporine using the oral solution once a day has been used.
Topical immunomodulators such as pimicrolimus and tacrolimus 0.1% ointment applied twice daily have also been helpful and avoid the risk of atrophy and striae, which are risks of long-term topical steroid use.4
Intralesional triamcinolone injections are an option for patients who do not respond to topical corticosteroids or topical immunomodulators, using a lower potency injection to avoid the risk of atrophy and striae.5
Botulinum toxin has been used (as in the treatment for hyperhidrosis), with benefit, in a small study, with no adverse effects.6
Local destructive measures—excision, carbon dioxide laser, split-thickness skin graft, and dermabrasion— have been used for chronic unresponsive areas.
Hailey-Hailey disease (HHD) has a chronic, relapsing, and remitting course. The long-term benefits of medical and/or surgical approaches to HHD are uncertain, and recurrence is common. Patients with HHD have a normal life expectancy, although with significantly impaired quality of life.7
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 177.
- Hohl D. Darier Disease and Hailey-Hailey Disease. Dermatology, edited by Jean Bolognia, Elsevier Limited, 2018.
- Zhang D, Li X, Xiao S, Huo J, Wang S, Zhou P. Detection and comparison of two types of ATP2C1 gene mutations in Chinese patients with Hailey-Hailey disease. Arch Dermatol Res. 2012 Mar;304(2):163-70.
- Tchernev G, Cardoso JC. Familial benign chronic pemphigus (Hailey-Hailey Disease): use of topical immunomodulators as a modern treatment option. Rev Med Chil. 2011 May;139(5):633-7.
- Hohl D. Darier Disease and Hailey-Hailey Disease. Dermatology, edited by Jean Bolognia, Elsevier Limited, 2018.
- Koeyers WJ, Van Der Geer S, Krekels G. Botulinum toxin type A as an adjuvant treatment modality for extensive Hailey-Hailey disease. J Dermatolog Treat. 2008;19(4):251.
- Morrell, D. Hailey-Hailey disease (benign familial pemphigus). UpToDate, 2022. www.uptodate.com