Introduction
Fox-Fordyce disease1 is an uncommon, very itchy, papular eruption of the axillary and anogenital regions, believed to be related to apocrine sweat duct occlusion.
Epidemiology
There is a 9-1 ratio of women to men who get this condition, which is more common in tropical areas. Exact incidence is unknown.
Etiology
The apocrine sweat gland ducts become plugged, resulting in papular inflammation. Rubbing and scratching to alleviate symptoms may make the condition worse.
Symptoms and clinical features
Itching and irritation in the vulvar area and axillae can be acute, intense, and sometimes cyclic. The itching may improve with pregnancy and oral contraceptives. This annoying condition starts in puberty and ends with menopause.<
Monomorphous, skin-colored to slightly hyperpigmented, dome-shaped folliculopapules are observed in the axillae and in the anogenital region, mainly involving the mons pubis and labia majora areas.
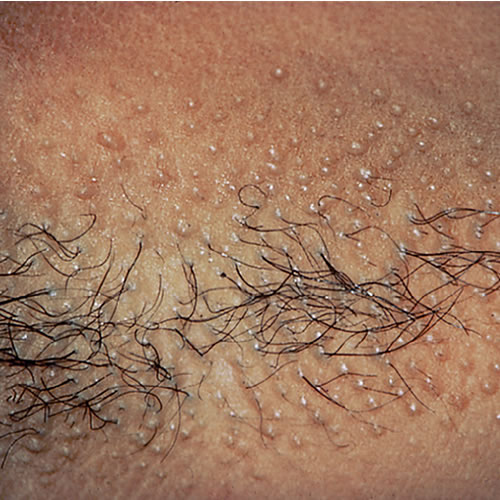
There is often a regular, cobble-stoned appearance to the papules.
Diagnosis
Clinical presentation and biopsy define the diagnosis.
Pathology/Laboratory Findings
Biopsy can help with diagnosis.
Differential diagnosis
Differential diagnosis includes syringomata and folliculopapular lichen simplex chronicus
Treatment/management
Local. Cold gel packs are useful when the patient’s itching is intense. Pramoxine HCl 1%, menthol 1⁄4%, camphor 1⁄4% in a cream base 3 to 4 times a day can be used as a non-specific antipruritic.
Specific Treatment. Oral contraceptives can be very effective. Hydrocortisone 1% cream or ointment with 1⁄4% camphor used two to three times a day as needed, is prescribed for mild cases. Super potent corticosteroids, for example clobetasol or halobetasol 0.05% cream or ointment, twice a day for 10 to 14 days intermittently may be needed for resistant cases. Caution the patient that overuse can cause thinning of the skin. Topical Tretinoin (Retin-A) 0.025% or 0.05% cream is another alternative provided there is no excessive irritation.
For severe cases, surgical excision is an option of last resort.