Introduction
Crohn disease1 is a chronic, granulomatous, inflammatory bowel disease that, rarely, can involve the vulva and groin, either primarily or secondarily.
Epidemiology
Crohn disease commonly occurs between the ages of 20 to 30 years with a prevalence rate of 100 to 200 per 100,000. Of women with Crohn disease, 2% have associated vulvar involvement, although this number may be unrealistically low due to inadequate diagnosis.
Etiology
The etiology is unknown. Proposed causes include an unrecognized infectious agent or a disturbed immunologic reaction to an intestinal organism in a genetically predisposed individual. It is unclear whether the inflammation represents a primary immunodeficiency or and autoimmune reaction.2
Symptoms and clinical features
The cutaneous changes associated with vulvar Crohn Disease can occur years before the onset of bowel symptoms, characteristically with knife-like fissures in the labiocrural folds with an absence of inguinal lymphadenopathy. In addition, patients may complain of painful or painless, unilateral or bilateral swelling of the labia, perianal skin tags, and perianal fistulas. Abscesses may also form, starting with nodules reminiscent of hidradenitis suppurativa.
Anogenital patterns of Crohn’s disease include the following:
- Contiguous: in this form there is a direct extension from the involved intestine with the formation of sinuses/fistulae to the skin or other organs
- Metastatic (noncontiguous): very rare, with ulcers and swelling in the vulvar area, distant from the intestinal manifestations
- Non-Specific mucocutaneous lesions: aphthous ulcers, pyoderma gangrenosum
The patient may present with painful, thickened swelling of the vulvar or perianal area with or without draining sinuses (fistulous tracts). If present, these tracts may or may not connect directly to the gastrointestinal tract. Simple painful swelling may be the sole complaint, but ulcerated lesions cause pain and dyspareunia. Early disease may present with painless swelling.
Labial edema may be localized or generalized and may or may not be inflammatory.
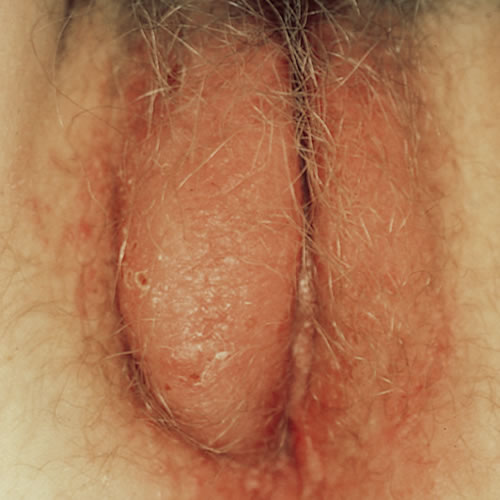
The severity of erosions and ulceration varies. As stated above, the classic ulcerations associated with this condition are called “knife cut” linear fissures and are located along the labiocrural fold.
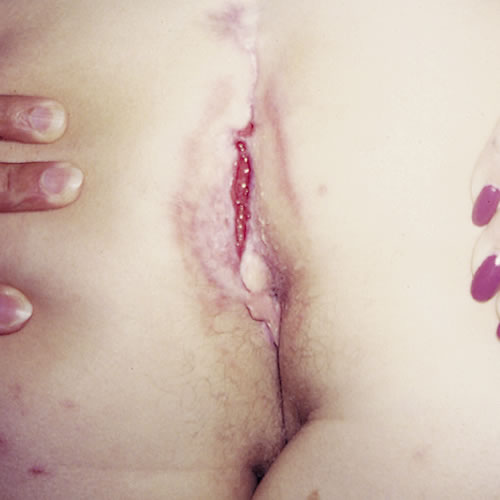
The ulcers may be solitary, deep, and necrotic and may lead to fistulae.
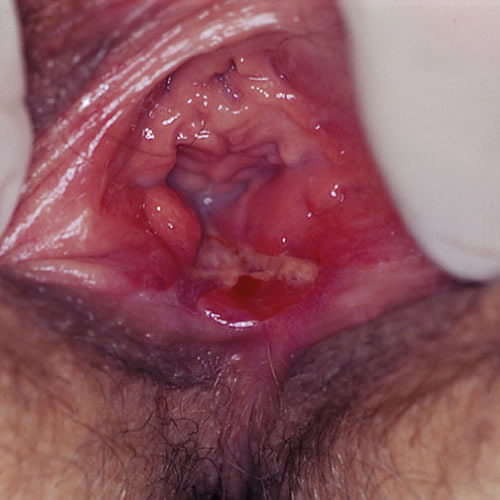
The area of involvement may extend to the perineal and perianal area.
Diagnosis
The diagnosis is usually clinical, especially in the case of known intestinal disease. Biopsy shows typical granulomatous change, though diagnosis may be non-specific in the pathology report.
Pathology/Laboratory Findings
Biopsy is helpful in identifying the typical granulomatous changes. If intestinal disease has not yet been diagnosed, endoscopic or radiologic testing should be recommended, as intestinal disease may be, as yet, asymptomatic.
Differential diagnosis
Hidradenitis suppurativa, Behçet disease, lymphogranuloma venereum, granuloma inguinale, and genitourinary tuberculosis. In a patient with biopsy-proven granulomatous vulvitis, consider Crohn disease.
Treatment/management
Treatment depends on the extent of involvement of the perianal area and the associated bowel disease. A team consisting of a dermatologist, gynecologist, and gastroenterologist is needed to successfully manage the condition. Intestinal disease should be treated appropriately but treatment may or may not affect anogenital disease. There is a possibility of squamous cell carcinoma developing in untreated lesions.3 Treatment usually involves systemic corticosteroids, methotrexate, sulfasalazine or metronidazole used individually or in combination.4 These medications should be prescribed by the clinician with the most appropriate expertise according to the needs of the patient, and in consultation with other members of the clinical team.
When bowel disease is not active and the problem is the vulvar ulcers and edema, the following treatment can be used:
General care: Warm sitz baths followed by patting dry, application of petrolatum as needed for barrier function, avoidance of irritants and tight clothing. Topical xylocaine 5% may be used for pain.
Topical steroids must be super potent: Clobetasol or Halobetasol 0.05% ointment applied twice a day. A bland barrier ointment or paste such as Zinc Oxide can be used for protection.
Intralesional triamcinolone (Kenalog-10) diluted 1:1 with saline injected using a 30-gauge needle is useful for small ulcers, erosions, and swollen granulomatous areas.
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc., 1998. 161-163.
- Coulombe F, Behr MA. Crohn’s disease as an immune deficiency? Lancet 2009; 374:769-70.
- Edwards L and Lynch P. Genital Dermatology Atlas, second edition. Lippincott Williams and Wilkins, 2011. 173.
- Baumgart DC, Sandborn WJ. Inflammatory bowel disease: clinical aspects and established and evolving therapies. Lancet. 2007;369: 1641-1657.