Introduction
With the gradual loss of serum estrogen as women age, the epithelium of the vulva and vagina undergo atrophy (thinning of the tissue).1 In post-menopausal women, this is responsible for many of the symptoms of Genitourinary Syndrome of Menopause (GSM).2 Other low estrogen states such as the postpartum period and lactation, as well as premature or artificial menopause and the use of anti-estrogen drugs, can produce the same effects, in some cases temporarily. In the reproductive years, the vaginal epithelium is rugated and glycogen-rich, with high collagen content. The vaginal environment is acidic, with the pH usually less than 4.5, and normal flora protect the tissue. Normal vaginal secretions provide moisture and lubrication. The vulvar tissue is plump and the epithelium resilient.
With estrogen loss, the vestibular and vaginal mucosa reddens, then turns pink, then develops pallor. Pigmentation fades. The labia majora atrophy and in thin women can become floppy; the labia minora can almost disappear (though dermatosis must always be ruled out if normal anatomy is missing). The clitoris may appear somewhat larger due to a relative increase in androgens and decrease in prepuce covering. Aging and multiple deliveries produce a weakening of the muscular structures, resulting in a tendency toward prolapse of the urethra, bladder, uterus, vagina, and rectum. The vaginal epithelium thins and loses elasticity. There can be shortening and narrowing of the vaginal canal (though, again, other conditions that cause shortening and narrowing need to be ruled out). There is a decrease in vaginal secretions and vaginal pH becomes elevated. Women who were previously comfortable with penetrative sex, complain of “dryness,” tightness of the introitus, bleeding, unusual discharge, sometimes odor, and/or dyspareunia.
Epidemiology
All women go through aging and eventual menopause. Not all women experience discomfort in the vulvovaginal area related to this, but a large number do. In a large multi-national survey, 39% of postmenopausal women complained of symptoms related to atrophy.3 Many are symptomatic but do not complain.
Etiology
The cause of atrophic vulvovaginal symptoms (GSM) is loss of estrogen resulting from menopause, castration, anti-estrogens (tamoxifen), or ovarian destruction. There is a relative estrogen deficiency before menarche, postpartum until the return of the menses, and during breast-feeding. In the very early months of breastfeeding, women may be disappointed to not be able to return to the sexual relationship they once had, but may attribute discomfort to having given birth. Later during lactation, complaints arise when the couple really expects to return to “normal,” but is not able to, although there is an increasing return to pre-pregnancy vaginal maturation index as time goes on. Premenarchal girls or young teenagers sometimes present with labial adhesions from their hypoestrogenized state that will respond to treatment with topical estrogen.
Natural menopause is the most common cause of vulvovaginal atrophy. With a thin, atrophic, vaginal epithelium, there is a shift in vaginal pH with values from >4.5 up to 7, and a shift in the vaginal maturation index from the superficial epithelial cells and robust lactobacilli of premenopause, to a preponderance of parabasal cells and absence of lactobacilli. Overgrowth of normally commensal organisms may occur, with resulting infection, adding to discomfort.
Symptoms and clinical features
Patient history includes complaints of vulvar burning, dysuria, pruritus, tenderness, and dyspareunia. Women often complain of vaginal “dryness.” A watery, scalding discharge may occur. There may be exquisitely painful fissures, with slight bleeding around the introitus. Pain and bleeding may occur with intercourse alone, while the woman is comfortable day to day.
The vulvar trigone may be pallid. The vagina may be pale or erythematous, the vaginal walls smoother, and the tissues thinner.
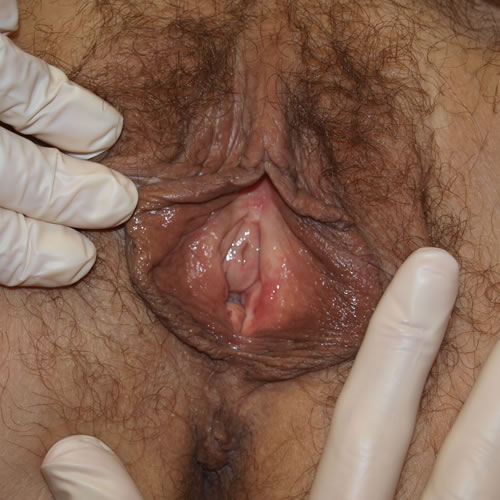
There may be introital stenosis. Petechiae and fissures may be seen. The discharge may be heavy, malodorous, gray, yellow, or even green in color, with a pH of 6 to 7 or there may be no discharge and scanty secretions. Urethral caruncles (seen as smooth, red tissue at the opening of the urethra), urethral prolapse, or polyps may occur.
Use of even the thinnest speculum may cause pain and bleeding. The vagina may appear to be foreshortened.
Diagnosis
Diagnosis is made clinically based on history, physical exam, and use of the maturation index via vaginal pH and wet prep with microscopy.
Pathology/Laboratory Findings
Vaginal pH and wet prep are performed. Cellular material for analysis may be scanty as secretions may be reduced. The vaginal pH is elevated (>4.5, usually in the 5.5-7.0 range). On saline wet prep, there is a preponderance of parabasal cells rather than the tough, superficial squamous epithelial cells that are a sign of adequate, protective epithelium. There is an absence of lactobacilli. White blood cells may or may not be present. There may be overgrowth of other organisms: gram-negative rods and gram-positive cocci. (Microscopy Tables)
Differential diagnosis
One must make sure of the diagnosis. Postmenopausal bleeding, if from the uterus or an unknown source, needs to be assessed with endometrial biopsy and pelvic ultrasound. Women whose symptoms are related to urination (frequency, urgency, dysuria) need to be assessed for urinary tract infection or other conditions of the bladder. Women with pelvic organ prolapse who may try pessaries will benefit from the effects of topical estrogen prior to and during pessary treatment if there are no contraindications. Often, a wet prep that looks like bacterial vaginosis or non-infectious vaginitis (desquamative inflammatory vaginitis) will revert to normal (premenopausal characteristics) with estrogen treatment alone.
Lichen planus can cause distortion of normal tissue and patches of erythema (erosions) in the vestibule. Concomitant conditions should always be looked for.
Treatment/management
- Avoid irritating soaps and hygiene products.
- Cleanse gently with Dove or other mild soap.
- Use lubricants and emollients. Plain Vaseline applied to vulvar tissue in a thin film after showers can keep the skin supple.
- Lubricants include Astroglide and Slippery Stuff or a tiny amount of plain vegetable oil. There are commercial emollients and lubricants which can be used if they don’t bother the skin. Sexual activity may promote increased elasticity and fewer symptoms, but will be impossible if too much pain is present.
- Treat intercurrent infections.
- Treatment of atrophy with estrogen is more effective than emollients and lubricants alone in improving symptoms. Estrogen restores low pH and lactobacilli, thickens the epithelial tissue, increases natural lubrication and improves bladder or urethra-related symptoms.4For treating atrophy alone, (not vasomotor symptoms or bone loss), topical preparations are completely adequate and give the woman the lowest possible exposure to estrogen. If a patient is taking oral hormone replacement therapy, she may still need topical estrogen in the vestibule to have pain-free sex. The lowest possible doses should always be used, within the context of the woman’s preferences. As long as the manufacturer’s directions for dose are adhered to, concurrent progestin is not needed. 5
- Women with breast cancer may use topical vaginal estrogen if approved by their oncologists. Use of topical vaginal estrogen in women taking Tamoxifen or aromatase inhibitors may not be recommended simply because the effect of any additional absorption of estrogen on estrogen-dependent tumors, however small, in these patients is unknown.6 7 (Annotation P: Vaginal secretions, pH, microscopy, and cultures, Section on Vaginal Atrophy.)
Occasionally, additional treatment with pelvic floor physical therapy may be useful in women who have vulvodynia despite improvement in the vaginal environment with topical estrogen treatment. Topical xylocaine 5% ointment applied about 10-15 minutes prior to attempt at vaginal penetration, left on for at least five minutes and then wiped off prior to application of lubricant, may be helpful in some women.
Table P-18: Local treatment of vaginal atrophy with estrogen, lowest to highest doses
| Vagifem (or Yuvafem) tablets, 10 mcg intravaginally nightly for 14 days, then twice weekly (total 20 mcg/week) |
| Estring, vaginal ring, 7.5 mcg/24 hr inserted vaginally once every 90 days (total 52.5 mcg/week) |
| Premarin cream, (0.625 mg conjugated estrogens/1 g cream): 0.5 gm intravaginally, nightly for seven days, then twice weekly (total 600 mcg/wk) |
| Estrace cream, (100 mcg estradiol/1 g cream): 0.5 gm intravaginally, nightly for seven days, then twice weekly (total 100 mcg/wk) |
References
- Fisher BK, Margesson, LJ. Genital Skin Disorders: Diagnosis and Treatment. Mosby, Inc.,1998. 106-107.
- Portman DJ, Gass MLS. Genitourinary Syndrome of Menopause: new terminology for vulvovaginal atrophy from the International Society for the Study of Women’s Sexual Health and the North American Menopause Society. Menopause: JNAMS, 2014;21(10) 1063-8.
- Nappi RE, Kokot-Kierepa M. Women’s voices in the menopause: results from an international survey on vaginal atrophy. Maturitas. 2010; 67:233.
- Srinivasan S, Hua X, Wu MC, Proll S, Valint DJ, Reed SD, Guthrie KA, LaCroix AZ, Larson JC, Pepin R, Bhasin S, Raftery D, Fredricks DN, Mitchell CM. Impact of Topical Interventions on the Vaginal Microbiota and Metabolome in Postmenopausal Women: A Secondary Analysis of a Randomized Clinical Trial. JAMA Netw Open. 2022 Mar 1;5(3):e225032. doi: 10.1001/jamanetworkopen.2022.5032. PMID: 35353163; PMCID: PMC8968546.
- Bachman G, Bouchard C, Hoppe D, et al. Efficacy and safety of low-dose regimens of conjugated estrogens cream administered vaginally. Menopause. 2009; 16:719.
- Al-Baghdadi O, Ewies AA. Topical estrogen therapy in the management of postmenopausal vaginal atrophy: an up-to-date overview. Climacteric 2009; 12:91.
- Kendall A, Dowsett M, Folkerd E, Smith I. Caution: Vaginal estradiol appears to be contraindicated in postmenopausal women on adjuvant aromatase inhibitors. Ann Oncol 2006; 17:584.